Management of chronic type B aortic dissection
Abstract
The standard of care first-line therapy for uncomplicated acute type B aortic dissection is medical therapy. As a result, many of these dissections progress to become chronic type B aortic dissections (CTBAD). In the following manuscript, we will outline the natural history of these lesions and review what constitutes a CTBAD by anatomy and chronology. We will also describe the long-term medical management and surveillance of these lesions, what constitutes high-risk features, and when intervention should be considered. Endovascular, open and hybrid management strategies, potential complications, and subsequently required surveillance will also be discussed. With proper medical management, surveillance, and intervention, CTBAD can be managed effectively and downstream morbidity minimized.
Keywords
INTRODUCTION
Aortic dissection affects approximately 30 people per million individuals per year[1]. This life-threatening event occurs when the intimal lining of the aorta is disrupted, and blood can separate the fibers of the aortic media, propagating the lesion. Dissections are classified according to the location of the intimal tear and the affected segments. The prognosis and treatment of these lesions differ depending on the anatomic classification. The prognosis is also affected by the time since the inciting aortic event, as certain problems can occur acutely, while different issues arise in the chronic phase. In this manuscript, we will focus on chronic aortic dissections that involve the aorta distal to the left subclavian artery (type B).
In the past, open surgical management was the treatment of choice when intervention was required for chronic type B aortic dissections (CTBAD). In 1999, endovascular stent grafting was first reported as a therapy for this disease process. Since then, thoracic endovascular aortic repair (TEVAR) has become an important component in the management of CTBAD, either as a stand-alone therapy or combined with open surgery in a hybrid manner[1,2]. Life-long clinical and imaging surveillance of patients with known aortic dissection is necessary to identify those who may require intervention to prevent aortic catastrophe, as well as to monitor for complications after a successful repair. In this manuscript, we will review the classification, natural history, and imaging strategies for CTBAD, as well as describe the options available for intervention to address these lesions.
CHRONIC TYPE B AORTIC DISSECTION
Anatomic classification
The original classification system proposed by DeBakey in 1965 was based on the longitudinal extent of the anatomic involvement. A type I dissection involved the ascending aorta and descending aorta. A type II involved the ascending only. A type IIIA involved only the descending thoracic aorta, while a type IIIB involved both the thoracic and abdominal aorta distal to the left subclavian artery[3]. The more commonly used classification system is the Stanford Classification developed in 1970, in which dissections that involve the ascending aorta are grouped as type A, and those not involving the ascending aorta are grouped as type B[3]. This classification system gained popularity over the DeBakey classification due to its simplicity and its use in the International Registry of Acute Aortic Dissections (IRAD) database[4]. However, the Stanford system lacks a description of the longitudinal extent of the dissection and details about the location of the entry tear. Furthermore, neither classification scheme addresses dissections that originate in the arch.
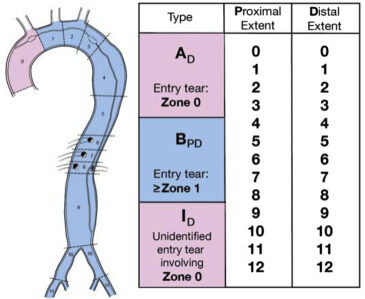
Because the management of dissection differs greatly depending on the location of the entry tear, it is important to have an accurate classification scheme. For this reason, in 2020, the Society for Vascular Surgery (SVS) and The Society of Thoracic Surgeons (STS) issued a reporting standards document to clarify how lesions should be classified[3]. Per this consensus, the distinction between type A and type B dissection is predicated solely on the site of the entry tear. Any entry tear originating in Zone 0 of the aorta is a Type A#, with a subscript numeral designating the distal extent of the dissection. Any dissection with entry tear in zone 1 or beyond is a type B#,# with two subscript numerals: the first designating the proximal extent of the lesion (e.g., retrograde involvement of the ascending), and the second numeral designating the distal extent of the dissection [Figure 1]. If there is zone 0 involvement, but the location of the primary entry tear cannot be determined, then it is type I# indeterminate, with the subscript numeral again designating the distal extent.
Figure 1. SVS/STS guidelines on anatomic reporting of dissections from Lombardi et al.[3] (with permission). SVS: Society for Vascular Surgery. STS: The Society of Thoracic Surgeons.
Chronologic classification
The reporting standards document issued by the SVS/STS also clarifies the way the chronicity of dissection is classified. This new classification system incorporates data from both IRAD as well the European Society of Cardiology. Dissections are considered: hyperacute, < 24 hours; acute, 1 to 14 days; subacute, 15 to 90 days; and chronic, > 90 days[3]. Of note, the definition of acute and chronic dissection has changed over time, and many studies in the literature published prior to this new classification will term dissections > 2 weeks from the inciting event as chronic[1,4]. Thus, it is important to clarify how the term chronic was defined when comparing studies.
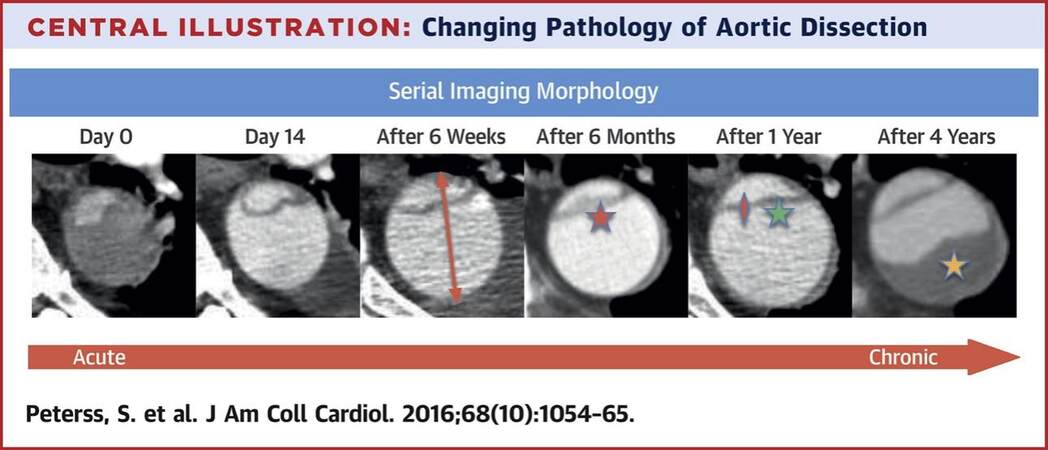
Distinguishing the chronicity of dissection can sometimes be aided by cross-sectional imaging. Typical features of a more acute process on CT include periaortic confluent soft tissue opacity, and a curved and mobile dissection flap[5]. Features more suggestive of a chronic dissection include a thick flap, false lumen outer wall calcification and thrombus, false lumen dilatation, and tear edges curling in to the false lumen[5]. Figure 2 demonstrates the changing pathology of aortic dissection in a patient longitudinally over 4 years[6].
Figure 2. Changing temporal pathology of aortic dissection, from Peterss et al.[6] (with permission).
Natural history
Type B dissections represent 25%-40% of all dissections[4]. The leading cause of death in patients with acute type B dissection is aortic rupture, and the second leading cause of death is malperfusion[7]. Fortunately, 91% of patients with acute Type B aortic dissection will survive the initial event. Of these survivors, 66% will have an initially uncomplicated course with proper medical management (see Medical Management). While not all will require intervention, 60% of survivors will develop late aneurysmal dilation of the affected segment(s) of the aorta over the next five years[8]. This dilation tends to predominantly affect the upper descending thoracic aorta adjacent to the primary tear but can affect the abdominal and visceral segments as well[7]. Dissected descending thoracic aortas tend to grow at a rate faster than aneurysms of the ascending and abdominal aorta. Additionally, the greater the size of the aorta, the faster it grows[9]. As with atherosclerotic aneurysms, size plays a major role in the risk of rupture. Aneurysmal dilation > 6 cm carries a yearly rupture rate of 6.9%, and repair should be considered as this size is approached[10]. Once 7 cm in size is reached, the lifetime rupture risk is 43%[9].
The growth of a CTBAD can vary from 0.1 cm to 0.7 cm per year but is strongly dependent on the initial aortic size and control of hypertension[9]. Despite optimal medical management, at least one-third of patients will require surgery for aortic-related complications within five years of the dissection event, with the greatest risk being in the first few months[2].
After an intervention on CTBAD, positive or negative aortic remodeling can be detected with imaging. Positive aortic remodeling in a segment of the aorta is defined as any one of the following: reduction in false lumen diameter/volume with no change in total aortic diameter/volume; true lumen diameter/volume expansion with no change in total aortic diameter/volume; or total aortic maximal diameter reduction with variable changes in true and false lumen diameters. Negative aortic remodeling would represent the opposite observation. It should be noted that reporting on aortic remodeling should include the entire dissected aorta, as one may see positive remodeling in one segment (e.g., proximal thoracic) and negative remodeling in another (distal thoracic, visceral, abdominal, iliac)[3].
Medical management
The cornerstone of chronic medical therapy for CTBAD is “anti-impulse therapy”, with beta-blockers as a first-line agent[7,11]. Beta-blockers reduce the force of left ventricular contraction and thus attenuate aortic wall stress[12]. Studies have shown that long-term treatment with beta-blockers reduces the progression of aortic dilation, incidence of hospital admission, incidence of late aortic procedures, and cost of therapy when compared with other (non-beta-blocker) antihypertensive agents[11]. Target parameters should include blood pressure no greater than 140/90 mmHg, or 130/80 mmHg in patients with diabetes or chronic kidney disease (according to European and North American guidelines)[12-14]. Other medications such as calcium channel blockers and renin-angiotensin-aldosterone system modulators can be used in patients who are refractory to or intolerant of beta-blockers[12]. Angiotensin receptor blockers may be particularly useful in patients with Marfan or Loeys-Dietz syndrome[13].
As many of these patients have concomitant cardiovascular disease, encouraging exercise, weight reduction, smoking cessation, and initiating antiplatelet therapy as needed is important in reducing cardiovascular morbidity[12]. Statins should be used with a target low-density lipoprotein profile of less than 70 mg/dL in patients at risk of coronary artery disease. Other studies have shown that maintaining an optimal lipid profile with the use of statin medications can also promote favorable aortic remodeling[15].
Surveillance and imaging modalities
Aortic dissection results in varying degrees of ongoing and permanent injury to the aortic wall, and thus lifelong follow-up is required[2]. A family history of unexplained death, bicuspid aortic valve, aortic dissection, or aortic aneurysm should trigger genetic testing and family counseling[12]. The period of greatest risk for aortic complications after acute dissection is near the index event, and thus intervals of 30 days, 3 months, 6 months, and yearly thereafter are recommended for follow-up imaging, although this may vary based on individual patient circumstances[2,3].
The morphology of the dissected aorta will change over time. As remodeling occurs, the dissection may extend into new aortic zones or regress out of previously injured zones, and the extent of the disease burden should be updated using the SVS/STS classification system[3]. The important parameters to document are total aortic diameter, true lumen and false lumen diameter, distal entry tears, and the status of the false lumen, including whether it is patent, partially thrombosed, or completely thrombosed[3]. Multiphase computed tomography angiography (CTA) is the imaging modality of choice for CTBAD due to its sensitivity for detection of false lumen flow, false lumen thrombosis, changes in aortic diameter, and prior treatment/device complications[3]. Delayed contrast phase imaging is important to reveal any delayed false lumen perfusion by distal fenestrations[16,17]. Other imaging modalities such as magnetic resonance angiography and echocardiography may also be considered in select patients[12].
Indications for surgical intervention
Any consideration of intervention on the aorta must balance the patient’s life expectancy versus the risk of the procedure. For most patients, an aneurysm of the descending thoracic aorta > 5.5 cm warrants intervention. This is based on data demonstrating that 23% of patients with rupture of a chronically dissected aorta had an aortic dimension between 5 and 6 cm, with a median last known aortic diameter of 5.4 cm[18,19]. This size criterion may be adjusted based on the size of the patient and the size of their normal contiguous aorta, and typically an aneurysm more than twice the size of the normal contiguous aorta should be considered for replacement[9].
Indications for intervention at smaller sizes may include rapid growth of the aneurysm (> 5 mm -10 mm in 12 months) or a saccular aneurysm protruding 2 cm or more beyond the aortic wall[2]. Connective tissue disorder, family history of aortic catastrophe, contained aortic rupture, penetrating aortic ulcer, mycotic aneurysm, or new acute on chronic dissection may also warrant intervention at smaller sizes[9]. Symptomatic aneurysms should be treated regardless of size because symptoms typically herald impending rupture[9].
Surgical management
CTBAD may be treated by endovascular, open surgical, or hybrid approaches. Regardless of the strategy, common goals include limiting the extent of the aorta that is repaired to minimize associated morbidity, maintaining end-organ perfusion, and reducing the risk of dissection-related death[9]. The way these goals are achieved differs between endovascular and open surgical management. The objective of open surgical management is to replace the aneurysmal segment of the aorta. The objective of endovascular intervention is to cover the false lumen entry tears and promote false lumen thrombosis and positive aortic remodeling[2,20].
Deciding which intervention strategy to choose requires careful consideration of the anatomic features of the dissected aorta, including the site of entry tears, longitudinal extent of involvement, locations of fenestrations and branch vessels, as well as patient co-morbidities and life expectancy[4,9].
Patients being considered for open surgery to repair a descending thoracic aneurysm (DTA) or thoracoabdominal aortic aneurysm (TAAA) because of a CTBAD must have a thorough assessment by an experienced surgeon, preferably at a center of excellence/aortic referral center with high volume experience in performing these complex procedures. Consideration of patient age, co-morbidities, symptomatology, life expectancy, quality of life, aneurysm morphology and extent, and operator experience are all important considerations[9]. Open TAAA repairs are among the most anatomically violating and physiologically insulting surgical procedures performed in the modern era, with a 1-year morbidity and mortality of 17%-20%[21]. Due to the nature of the operation, the abdominal organs and spinal cord are exposed to a period of ischemia, making them vulnerable to injury[21]. Additionally, the unique combination of the thoracoabdominal incision and the necessity for single-lung ventilation make preoperative pulmonary function assessment particularly important[21]. Every effort should be made to medically optimize a patient prior to this intervention, and all organ systems should be evaluated. Echocardiogram, electrocardiogram, right and left heart cardiac catheterization, pulmonary function testing, complete metabolic panel and liver function testing, and CTA of the entire arterial tree are just a few of the preoperative tests that may be necessary[22]. Patients with prior abdominal or retroperitoneal surgery, large abdominal hernia, morbid obesity, and poor cardiopulmonary reserve are often unfit for open DTA or TAAA repair. While TAAA repair falls outside of the scope of STS preoperative risk calculator, this tool may be used to quantify patient co-morbidities.
TEVAR may offer a less morbid procedure and has been shown to be durable in the mid-term[23]; however, the long-term durability of these devices is unknown. Ideal candidates for TEVAR have the aneurysmal component limited to the descending aorta with the entry tear distal to but not involving the left subclavian artery[2]. Patients with a distal descending diameter of > 4.2 cm at the celiac axis are generally not candidates for standard TEVAR[2]. In a study of TEVAR for CTBAD, a 15% incidence of complete resolution of the thoracic and abdominal false lumen was observed in those treated with TEVAR. It should be noted that all these patients with complete false lumen resolution had the four visceral vessels fed by the true lumen and less than three distal (abdominal, iliac) residual fenestrations[24]. Greater than five distal fenestrations in the abdominal aorta and iliac arteries increase the risk for late aneurysmal degeneration of the abdominal aorta, even after treatment[24]. These anatomical features are therefore critical when considering which intervention strategy to offer. A tortuous and angulated aorta, or small and heavily calcified common femoral and iliac arteries, may also exclude TEVAR as an option. Occasionally an iliac or abdominal aortic conduit may be required for access[23].
Endovascular intervention
If TEVAR is planned for CTBAD, it is important to consider the proximal and distal landing zones, the extent of the aorta to be covered, and the access vessels. Proximally, a 2 cm landing zone proximal to the primary tear is desired. Although the proximal landing zone ideally should involve non-dissected aorta, the procedure can still be successful in many cases if a portion of the proximal landing zone is dissected, as may be seen in the case of a primary tear distal to the left subclavian artery. The average diameter measured via centerline technique in the undissected segment should be used to size the proximal portion of the endograft[2]. If required for adequate sealing, the origin of the left subclavian can be partially or fully covered and selectively revascularized based upon whether there is the preservation of pulsatile antegrade flow[2,25-27]. The location of distal fenestrations by thin-cut CTA should be studied preoperatively, and intravascular ultrasound (IVUS) can be useful for identifying them intraoperatively.
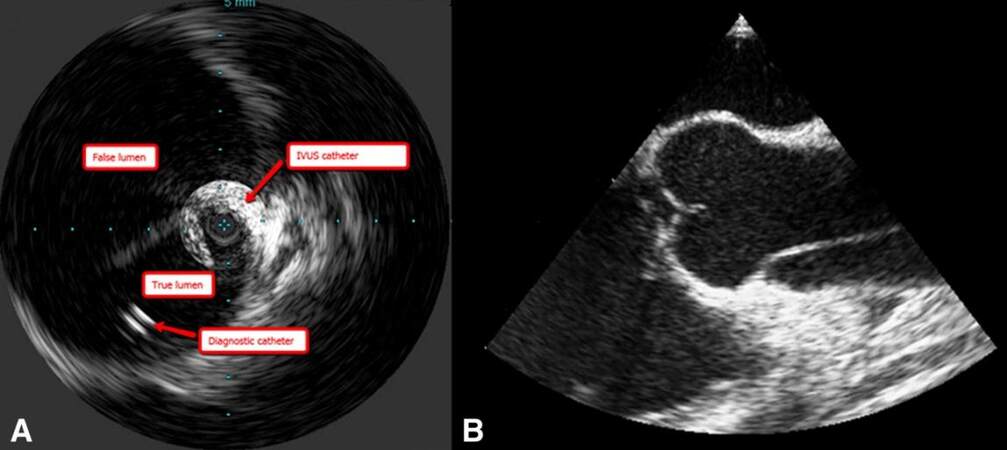
Operators should have a low threshold to cover the entire descending thoracic aorta down to the level of the celiac axis to eliminate distal fenestrations. In contradistinction to the proximal landing zone, the distal landing zone should be sized only to the true lumen to avoid stent graft-induced new entry tear (SINE) from excessive device oversizing relative to the small distal true lumen. Unlike acute type B dissection, where endograft deployment is always proximal to distal, in the setting of CTBAD, endograft deployment is often distal to proximal (so-called “distal first technique”). Larger proximal endografts can be placed to overlap inside distal smaller segments to minimize the risk of SINE[2,4,28]. CTA imaging can help guide the choice of access site, and IVUS is indispensable in confirming wire access of the true lumen[2]. Intraoperative transesophageal echocardiography and IVUS also help to assess the position and expansion of the endografts after deployment and rule out complications such as retrograde type A dissection[2] [Figure 3].
Figure 3. A: Use of IVUS in confirming wire access of the true lumen during TEVAR for a chronic type B dissection. B: TEE appearance of a retrograde type A dissection involving the ascending aorta. IVUS: Intravascular ultrasound; TEVAR: thoracic endovascular aortic repair; TEE: transesophageal echocardiography.
In stable patients with type B aortic dissection, several large studies have sought to determine whether intervention with TEVAR has benefit, and at what point in the disease process intervention should be performed. In the Investigation of Stent Grafts in Aortic Dissection (INSTEAD) trial, 140 patients with stable type B aortic dissection were randomized to optimal medical therapy (OMT) or OMT plus TEVAR[29]. The chronicity of the dissection at the time of randomization ranged from 2 weeks-52 weeks, with the median being in the sub-acute phase at approximately 6 weeks. Over an initial follow-up period of two years, there was no difference in the primary endpoint of all-cause mortality with OMT vs. TEVAR plus OMT. There was, however, a clear difference in morphological evidence of aortic remodeling, described by the authors as true lumen recovery and false lumen thrombosis. This was assessed by serially measuring the true and false lumens at the level of the maximal aortic diameter and at the aortic hiatus. Remodeling occurred in over 90% of the patients who received TEVAR vs. only 19% of those who received only OMT[29].
In longer-term follow-up of the patients randomized in the INSTEAD trial, INSTEAD-XL demonstrated a statistically significant reduction in all-cause mortality, aorta-specific mortality, and disease progression in patients who received TEVAR plus OMT compared to OMT alone. The results argue that TEVAR should be considered as a prophylactic measure in stable type B dissection to improve long-term outcomes[30]. This study, however, did not provide insight as to when this intervention should be performed.
The five-year follow-up report of the Study of Thoracic Aortic Type B Dissection Using Endoluminal Repair (STABLE1) did seek to elucidate if the timing of endovascular intervention had an impact on all-cause mortality and aortic remodeling[31]. This single-arm, multicenter study prospectively recruited 86 patients with complicated type B dissection, of which treatment with endovascular stent grafting occurred in the acute phase in 55 patients and sub-acute phase in 31 patients. No patients had TEVAR performed in what would now be classified as the chronic phase of their dissection. Both groups demonstrated favorable clinical outcomes and improvements in aortic remodeling, but no significant difference was reported between the groups in terms of 30-day/five-year mortality or the degree of remodeling. Complete false lumen thrombosis was observed in 74.1% of acute and 58.8% of nonacute patients at 5 years[31].
Given that interventions in both INSTEAD-XL and STABLE were performed in the acute or sub-acute phase of the disease, they did not clarify if TEVAR would have the same benefit in patients with chronic dissection (who have stable and thickened dissection flaps and distal fenestrations that pressurize the false lumen). A small single-center study from Duke University placed implantable pressure monitors into the proximal thoracic false lumen at the time of TEVAR for CTBAD and demonstrated a significant reduction in pressurization of the proximal thoracic false lumen after primary tear coverage with TEVAR[17]. Other series from multiple centers have also demonstrated false lumen thrombosis and beneficial positive thoracic aortic remodeling when CTBAD is treated with TEVAR, with excellent procedural and survival outcomes. TEVAR has been shown to have a lower peri-procedure morbidity and mortality, albeit with a higher reintervention rate, when compared to open surgery[17,24,32-34]. These findings have also been confirmed in a large meta-analysis of open vs. endovascular intervention for CTBAD[20]. If false lumen perfusion persists after TEVAR, embolization and other endovascular occlusion procedures have been successful in promoting thrombosis of the false lumen[35].
Open surgical intervention
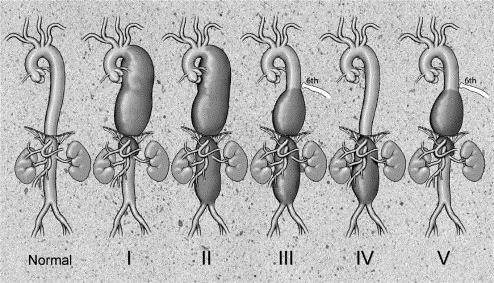
Open surgical intervention is the treatment of choice for patients with connective tissue disease or anatomy (typically TAAA) that is unsuitable for TEVAR[2]. The extent of the aneurysmal degeneration will determine the design of the operation needed for repair, and Dr. Stanley Crawford developed the currently utilized classification scheme of TAAA based upon the longitudinal extent of aneurysmal involvement[22]. Extent I TAAA spare the abdominal aorta, whereas extents II, III, and IV involve the abdominal aorta, with extent II being the most extensive [Figure 4]. The Safi modification adds type V, which extends from the distal thoracic aorta, including the celiac and superior mesenteric origins only (but not the renal arteries)[36].
Figure 4. Classification of thoracoabdominal aortic aneurysms. Extent I: distal to the left subclavian artery to above the renal arteries. Extent II: distal to the left subclavian artery to below the renal arteries; this is the most extensive type of aneurysm and the extent with the greatest risk of paraplegia as a complication of repair. Extent III: from below the sixth intercostal space to below the renal arteries. Extent IV: from below the twelfth intercostal space to the iliac bifurcation (total abdominal aortic aneurysm). Extent V: below the sixth intercostal space to just above the renal arteries. From Safi et al.[36] (with permission).
In the open approach, the aneurysmal segment of the aorta is ideally replaced from non-aneurysmal aorta proximally to normal caliber aorta distally, which may or may not be dissected. If dissection is present in the distal aorta at the anastomotic site, the distal dissection membrane may be fenestrated to allow perfusion of any branches being supplied by the false lumen. If no major branches rely on false lumen flow, the false lumen can be obliterated in the suture line. If dissected aorta remains after open repair, then the risk of subsequent aneurysmal degeneration distal to the anastomotic site remains as well[9]. In fact, even after open procedures, studies have shown 12% of patients require late additional intervention for subsequent aneurysmal degeneration[20].
Regarding the conduct of the operation, there are a wide variety of techniques and strategies available to accomplish the surgical resection safely. The simplest and oldest is the “clamp and sew” technique popularized by Dr. Stanley Crawford[22]. Due to the risk of organ ischemia, it has become widely accepted that intraoperative protection strategies should be considered in nearly all patients who are having an open repair of the DTA or TAAA[21-22]. These protection strategies include extracorporeal circulatory support, selective perfusion of visceral and large branch arteries, neurophysiologic intraoperative monitoring, and cerebrospinal fluid drainage[21].
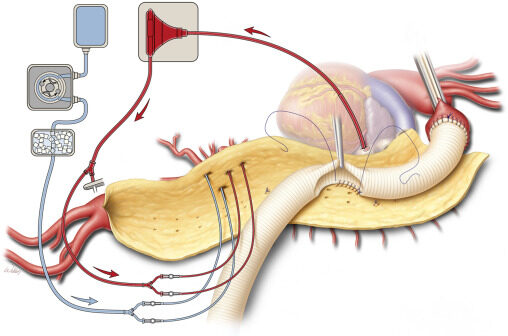
Extracorporeal circulatory support can be accomplished via left heart bypass (LHB), partial cardiopulmonary bypass (CPB), and full CPB with or without systemic cooling. The benefit of LHB is lower heparinization, but at the disadvantage of having to clamp the aorta to complete the proximal anastomosis, which may necessitate greater surgical dissection and risk damaging surrounding nerves and structures. Additionally, because the heart is relied upon to perfuse the upper body during LHB, systemic cooling cannot be initiated due to the risk of ventricular fibrillation. Individual perfusion catheters can be used in the ostia of the visceral vessels to maintain some organ perfusion during the period of visceral ischemia[22] [Figure 5].
Figure 5. Patch reattachment of intercostal arteries and cold renal perfusion and selective visceral perfusion during TAAA repair with LHB from Coselli et al.[22] (with permission). TAAA: Thoracoabdominal aortic aneurysm; LHB: left heart bypass.
Full CPB supplants the cardiac output, and it enables the operator to fully decompress the heat and cool the body for organ protection. Deep hypothermic circulatory arrest (DHCA) can then be used to complete the proximal anastomosis using an open technique if desired. Full CPB also allows the use of an oxygenator, which can be beneficial in patients with pulmonary disease, and cardiotomy suction to return lost whole blood to the circulation. The cost of full CPB is greater heparinization and thus more bleeding, as well as a rewarming period which may necessitate a longer bypass duration depending on the conduct of the operation. The full technical details of these various open surgical management strategies are beyond the scope of this paper, but are well described in the surgical literature[21,22,32,37]. A European study compared DHCA to LHB and found no difference in 30-day survival or major complications[37]. The most impactful procedural factor influencing patient outcome is the extent of resection[9] and likely surgeon experience[38].
At our institution, the preference is for full CPB with DHCA for all Extent II CTBAD TAAA cases, as well as Extent I cases involving the distal aortic arch, as this allows for a higher degree of organ protection and intraoperative flexibility and avoids the need for cross-clamp of the more proximal aortic arch. Additionally, we prefer direct distal aortic cannulation in this scenario rather than femoral arterial cannulation, to minimize the risk of retrograde embolization of chronic thrombus from the false lumen. We place preoperative lumbar drains the day prior to surgery in all patients with planned distal anastomosis below the level of T6[32]. Somatosensory and motor evoked potentials, as well as electroencephalography, are used for neurophysiologic intraoperative monitoring[39]. While other authors succeeded in using islands of the aorta to reimplant the visceral vessels[22], we prefer a side branch technique using a multi-branch Dacron graft to eliminate the risk of late patch aneurysm formation[39]. Dominant intercostal and lumbar arteries are reimplanted for spinal cord protection in nearly all cases using individual 8 mm side grafts to again avoid the risk of late patch aneurysm[21]. For Extent III and select Extent IV TAAA, including those developing late after prior TEVAR, we use LHB with full heparinization, which allows the use of an oxygenator and cardiotomy suction.
Hybrid intervention
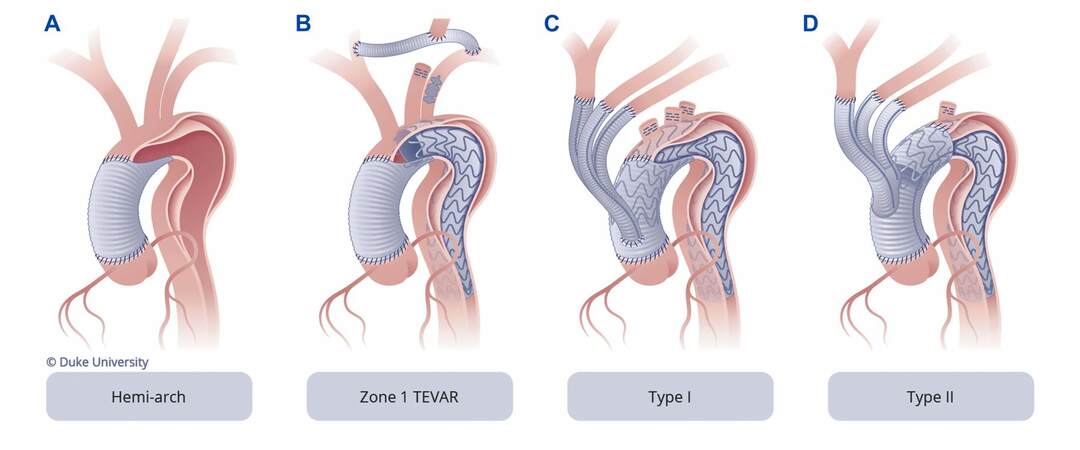
Hybrid procedures for CTBAD are diverse and can be tailored to the anatomy of a particular patient. Most commonly, disease in the ascending aorta and arch is treated with open surgery, followed by subsequent stent grafting of the remaining disease in the descending aorta. Procedures such as types I and II/III hybrid arch repair (HAR) [Figure 6] allow the extent of open surgical resection to be limited to the proximal aorta at the initial procedure, thus limiting the morbidity and allowing for a less invasive endovascular second stage, which avoids the risks of open DTA/TAAA repair[40]. The frozen elephant (FET) is another alternative and can be considered a variant of type III HAR[41]. It involves the replacement of the ascending aorta and part or all of the arch, with the deployment of a thoracic endograft into the DTA under HCA. The endograft is then incorporated into the distal anastomosis of the open surgical graft used to replace the arch[41]. This is all done in a single procedure and carries a risk of spinal cord ischemia of approximately 5% or higher in most series[42], which is the major disadvantage of the FET approach. However, our institutional preference is a staged approach utilizing type II HAR with first stage open proximal aortic repair followed by second stage completion TEVAR during a single hospital stay. This preference stems from the differing postoperative management strategies following open proximal aortic repair and TEVAR. Specifically, after open proximal aortic repair, lower blood pressures are preferred in the early postoperative period to reduce bleeding and anastomotic complications, whereas after TEVAR, higher pressures are preferred to optimize spinal cord perfusion pressure and minimize the risk of spinal cord ischemia[27,41].
Figure 6. Artist drawings of type I and II hybrid arch repairs (HAR) for chronic dissection. Type I: HAR involves debranching of the aortic arch vessels using a multi-branched Dacron graft sewn to either the native ascending aorta or, as shown in the drawing, a previously Dacron-replaced ascending aorta. This latter scenario is most commonly utilized in the setting of residual type B dissection after prior type A repair. Type II: HAR involves the replacement of the ascending aorta and, most commonly, a portion of the arch (to create proximal landing zone for the endografts) with distal anastomosis frequently in zones 1 or 2, along with debranching of the arch vessels.
Hybrid procedures may also be used to treat aneurysmal degeneration of the thoracoabdominal aorta. The visceral vessels are debranched via a laparotomy, and the thoracic and abdominal aorta are then treated with stent grafting[9,21,43,44]. This is a potential option for elderly and high-risk patients not suited to open repair and can be conducted in a staged fashion[44]. A previous study from our institution demonstrated no difference in the rate of paraplegia or 1-year mortality between hybrid and open TAAA repair, but with a higher rate of re-intervention and dialysis in the hybrid group[43]. Having the capability to perform a wide range of open and endovascular aortic interventions allows customization of the procedure to the needs and characteristics of the patient and their disease[40].
In the near future, physician-modified endografts (PMEGs) and visceral multi-branched endografts may become an alternative to hybrid abdominal debranching and TEVAR in unfit CTBAD patients with disease affecting the visceral segment; a prior small, single-institution study has confirmed the feasibility and short-term safety of PMEGs in the setting of chronic post-dissection TAAA[45]. Briefly, at our institution, the PMEG procedure involves the modification of an off-the-shelf endograft via the creation of 4 fenestrations corresponding to the patient’s anatomy based upon detailed measurements from the preoperative CTA study[46]. Patient selection for PMEG is critical. Specifically, suitable anatomy is paramount, as attempting to navigate a stiff small true lumen with branches originating from both lumens is a formidable technical challenge. The mid- and long-term outcomes of the procedure are unknown.
Complications
Open and endovascular interventions for CTBAD are not without risk. Potential complications are like those of any aortic surgery and include inducing new aortic dissection or rupture, stroke, bleeding, infection, acute kidney injury, bowel ischemia, and wound complications. The complication that is unique to aortic intervention is paraplegia due to spinal cord ischemia. The risk for spinal cord ischemia increases based on the length of the aorta covered/replaced, and the number of spinal cord feeding vessels that are sacrificed. This includes the vertebral, intercostal, lumbar, and internal iliac arteries. Neurophysiologic intraoperative monitoring with somatosensory and motor evoked potentials, as well as electroencephalography, can help to detect spinal cord and cerebral ischemia. Serial postoperative neurologic exams are also paramount to detect early evidence of proximal muscle weakness. Intra-operative measures to prevent or treat spinal cord ischemia include re-implantation of lumbar and intercostal branches in open surgery, or in endovascular surgery revascularization of any covered arteries such as the left subclavian artery, which is the major supply of collateral flow to the spinal cord[3,26,27].
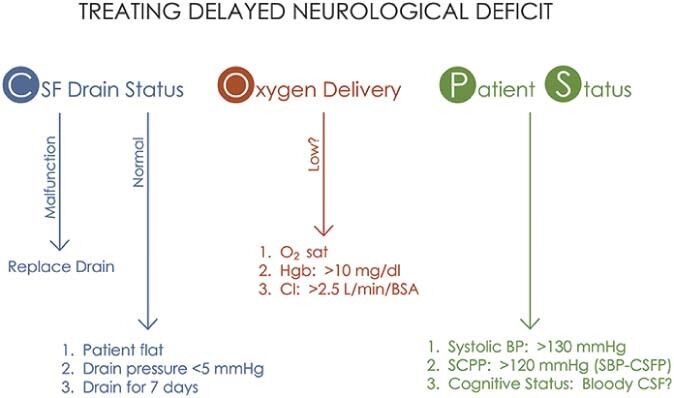
A systematic perioperative approach should be applied to manage any evidence of spinal cord compromise. The paraplegia treatment COPS protocol [Figure 7] is an example of this: with a focus on blood pressure stabilization, cerebrospinal fluid drainage, oxygen delivery, and patient status leading to an increase in spinal cord perfusion pressure[47]. Such standardization allows close monitoring and more rapid treatment of the factors influencing spinal cord ischemia.
Figure 7. The COPS protocol from Sandhu et al.[47] 2017 (with permission).
Complications unique to TEVAR include endoleaks (see Post Intervention Surveillance below) as well as SINE. SINE may occur proximally, causing pseudoaneurysm formation or retrograde type A dissection[48]. If SINE occurs distally, it results in continued pressurization of the false lumen. The overall reported incidence of SINE after TEVAR may be as high as 25%[28], with distal SINE representing the majority. These injuries are more common after TEVAR is performed for CTBAD and usually occur in a delayed fashion 12 months-36 months after the intervention[3]. Other risk factors include oversizing of the distal stent-graft relative to the smaller true lumen, connective tissue disease, shorter length (< 145mm) stent-grafts, and proximal to distal stent-graft implantation sequence in chronic dissection[28]. Long-term follow-up data of patients who had TEVAR for acute complicated type B dissection demonstrated up to 25% of patients may require re-intervention, although this did not affect late survival[23].
Post intervention surveillance
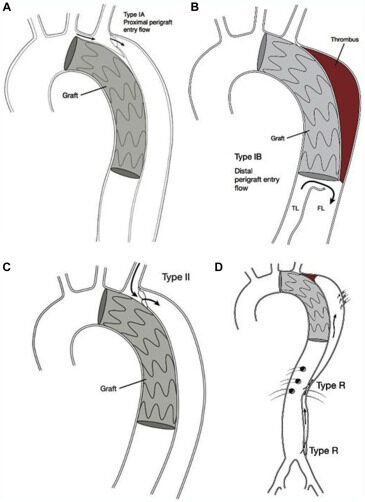
After an open or endovascular intervention, aortic surveillance should continue for the lifetime of the patient. As aneurysms may increase not only in diameter but also in length, the proximal and distal landing zones must be thoroughly examined for new pathology[9]. Persistent perfusion of the false lumen in both treated and untreated segments should be noted if it is present. This is classified differently than the typical endoleak classification scheme used for aneurysms: Type 1A entry flow is between the proximal endograft and the aortic wall; Type 1B entry flow is a distal entry tear adjacent to the endograft due to septal fenestration or SINE; Type II flow is retrograde flow through a branch artery; Type R entry flow is antegrade flow from the true lumen into the false lumen through distal septal fenestrations or branch vessels[3] [Figure 8]. A study of 4713 patients who had TEVAR for CTBAD showed that type IA, type IB, and type II endoleak each had a 1.6% incidence in this cohort at a median time of 239 days post-TEVAR[34].
Figure 8. (A) Type IA: entry flow is perigraft flow at the proximal edge of the stent graft that allows continued antegrade flow into the false lumen through the primary entry tear. (B) Type IB: entry flow is distal perigraft flow caused by a tear in the intimal membrane adjacent to the distal edge of the endograft [distal stent graft-induced new entry (SINE)] or an uncovered distal fenestration. FL: False lumen; TL: true lumen. (C) Type II: entry flow is continued retrograde false lumen perfusion through an arch branch (e.g., left subclavian artery as demonstrated in the illustration) or intercostal or bronchial artery. (D) Type R: entry flow is antegrade flow from the true lumen to the false lumen through septal, visceral, or distal fenestrations. From Lombardi et al.[3] (with permission).
CONCLUSION
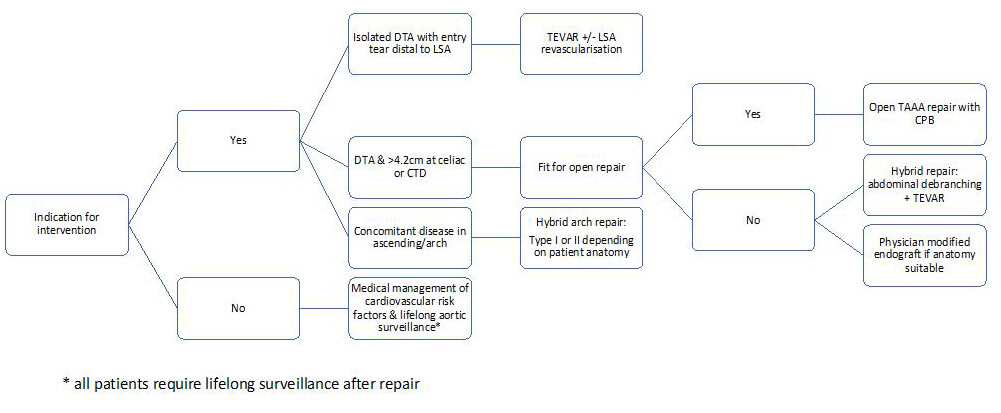
Type B aortic dissection is an evolving process that can continue to threaten the health of a patient well after it is first diagnosed. After 90 days from the inciting event, a dissection is designated as chronic, although the intimal flap and false lumen continue to evolve over time [Figure 2]. Patients with CTBAD should undergo systematic and lifelong screening to identify aortic complications requiring intervention. Aneurysmal degeneration above 5.5 cm generally warrants surgical intervention. Clinical trials have suggested that TEVAR may be an effective way to promote false lumen thrombosis and positive aortic remodeling. Not all aneurysms will be treatable with TEVAR, and some may necessitate open or hybrid surgery to repair, particularly those that involve the visceral segment or with retrograde arch involvement. [Figure 9] gives a summary of the treatment modalities for different situations potentially encountered with CTBAD. Patients should continue to have serial imaging even after repair of CTBAD to monitor for post-repair complications and development of metachronous pathology.
DECLARATIONS
Authors’ contributions
All authors contributed to the design, literature search, and writing of the manuscript.
Availability of data and materials
Not applicable.
Financial support and sponsorship
Not applicable.
Conflicts of interest
Dr. G. Chad Hughes is a consultant for Cryolife, Terumo Aortic, and W.L Gore and Associates.
Ethical approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Copyright
© The Author(s) 2022.
REFERENCES
2. Hughes G, Andersen ND, Mccann RL. Endovascular repair of chronic type B aortic dissection with aneurysmal degeneration. Operative Techniques in Thoracic and Cardiovascular Surgery 2013;18:101-16.
3. Lombardi JV, Hughes GC, Appoo JJ, et al. Society for vascular surgery (SVS) and society of thoracic surgeons (STS) reporting standards for type B aortic dissections. Ann Thorac Surg 2020;109:959-81.
4. Hughes GC. Management of acute type B aortic dissection; ADSORB trial. J Thorac Cardiovasc Surg 2015;149:S158-62.
5. Orabi NA, Quint LE, Watcharotone K, Nan B, Williams DM, Kim KM. Distinguishing acute from chronic aortic dissections using CT imaging features. Int J Cardiovasc Imaging 2018;34:1831-40.
6. Peterss S, Mansour AM, Ross JA, et al. Changing pathology of the thoracic aorta from acute to chronic dissection: literature review and insights. J Am Coll Cardiol 2016;68:1054-65.
7. Ziganshin BA, Dumfarth J, Elefteriades JA. Natural history of type B aortic dissection: ten tips. Ann Cardiothorac Surg 2014;3:247-54.
8. Fattori R, Montgomery D, Lovato L, et al. Survival after endovascular therapy in patients with type B aortic dissection: a report from the international registry of acute aortic dissection (IRAD). JACC Cardiovasc Interv 2013;6:876-82.
9. Svensson LG, Kouchoukos NT, Miller DC, et al. Society of Thoracic Surgeons Endovascular Surgery Task Force. Expert consensus document on the treatment of descending thoracic aortic disease using endovascular stent-grafts. Ann Thorac Surg 2008;85:S1-41.
10. Davies RR, Goldstein LJ, Coady MA, et al. Yearly rupture or dissection rates for thoracic aortic aneurysms: simple prediction based on size. Ann Thorac Surg 2002;73:17-28.
11. Genoni M, Paul M, Jenni R, Graves K, Seifert B, Turina M. Chronic β-blocker therapy improves outcome and reduces treatment costs in chronic type B aortic dissection. Eur J Cardiothorac Surg 2001;19:606-10.
12. Sabe AA, Hughes GC. Acute type B aortic dissection. Available from: https://books.google.com.hk/books?hl=zh-CN&lr=&id=kcPPDwAAQBAJ&oi=fnd&pg=PA487&dq=Sabe+AA,+Hughes+GC.+Acute+Type+B+Aortic+Dissection+53.&ots=wwD_MK5Sp8&sig=yrvRaevbeKWN17Xu-dK0IKHH4DE&redir_esc=y#v=onepage&q=Sabe%20AA%2C%20Hughes%20GC.%20Acute%20Type%20B%20Aortic%20Dissection%2053.&f=false [Last accessed on 20 Apr 2022].
13. Hiratzka LF, Bakris GL, Beckman JA, et al. American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. , American Association for Thoracic Surgery., American College of Radiology., American Stroke Association., Society of Cardiovascular Anesthesiologists., Society for Cardiovascular Angiography and Interventions., Society of Interventional Radiology., Society of Thoracic Surgeons., Society for Vascular Medicine. 2010 ACCF/AHA/AATS/ACR/ASA/SCA/SCAI/SIR/STS/SVM guidelines for the diagnosis and management of patients with Thoracic Aortic Disease: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines, American Association for Thoracic Surgery, American College of Radiology, American Stroke Association, Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, Society of Interventional Radiology, Society of Thoracic Surgeons, and Society for Vascular Medicine. Circulation 2010;121:e266-369.
14. Erbel R, Aboyans V, Boileau C, et al. ESC guidelines on the diagnosis and treatment of aortic diseases: document covering acute and chronic aortic diseases of the thoracic and abdominal aorta of the adult the task force for the diagnosis and treatment of aortic diseases of the European society of cardiology (ESC). Eur Heart J 2014;35:2873-926.
15. Tazaki J, Morimoto T, Sakata R, et al. CREDO-Kyoto PCI/CABG registry cohort-2 investigators. Impact of statin therapy on patients with coronary heart disease and aortic aneurysm or dissection. J Vasc Surg 2014;60:604-12.e2.
16. Hughes GC. TEVAR for chronic type B dissection: highlighting the importance of patient selection, adjunctive false lumen procedures, speaking the same language, and industry collaboration. Ann Thorac Surg 2021;111:501-2.
17. Parsa CJ, Williams JB, Bhattacharya SD, et al. Midterm results with thoracic endovascular aortic repair for chronic type B aortic dissection with associated aneurysm. J Thorac Cardiovasc Surg 2011;141:322-7.
18. Lansman SL, Hagl C, Fink D, et al. Acute type B aortic dissection: surgical therapy. Ann Thorac Surg 2002;74:S1833-5.
20. Boufi M, Patterson BO, Loundou AD, et al. Endovascular versus open repair for chronic type B dissection treatment: a meta-analysis. Ann Thorac Surg 2019;107:1559-70.
21. Parsa CJ, Hughes GC. Surgical options to contend with thoracic aortic pathology. Semin Roentgenol 2009;44:29-51.
22. Coselli JS, de la Cruz KI, Preventza O, LeMaire SA, Weldon SA. Extent II thoracoabdominal aortic aneurysm repair: how i do it. Semin Thorac Cardiovasc Surg 2016;28:221-37.
23. Hanna JM, Andersen ND, Ganapathi AM, McCann RL, Hughes GC. Five-year results for endovascular repair of acute complicated type B aortic dissection. J Vasc Surg 2014;59:96-106.
24. Hughes GC, Ganapathi AM, Keenan JE, et al. Thoracic endovascular aortic repair for chronic DeBakey IIIb aortic dissection. Ann Thorac Surg 2014;98:2092-7; discussion 2098.
25. Lee TC, Andersen ND, Williams JB, Bhattacharya SD, McCann RL, Hughes GC. Results with a selective revascularization strategy for left subclavian artery coverage during thoracic endovascular aortic repair. Ann Thorac Surg 2011;92:97-102; discussion 102.
26. Hughes GC. Commentary: left subclavian artery revascularization during zone 2 thoracic endovascular aortic repair: bypass versus transposition? J Thorac Cardiovasc Surg 2020;159:1228-30.
27. Weissler EH, Voigt SL, Raman V, et al. Permissive hypertension and collateral revascularization may allow avoidance of cerebrospinal fluid drainage in thoracic endovascular aortic repair. Ann Thorac Surg 2020;110:1469-74.
28. Hughes GC. Stent graft-induced new entry tear (SINE): intentional and not. J Thorac Cardiovasc Surg 2019;157:101-106.e3.
29. Nienaber CA, Kische S, Akin I, et al. Strategies for subacute/chronic type B aortic dissection: the Investigation of stent grafts in patients with type B aortic dissection (INSTEAD) trial 1-year outcome. J Thorac Cardiovasc Surg 2010;140:S101-8; discussion S142.
30. Nienaber CA, Kische S, Rousseau H, et al. Endovascular repair of type B aortic dissection: long-term results of the randomized investigation of stent grafts in aortic dissection trial. Circ Cardiovasc Interv 2013;6:407-16.
31. Lombardi JV, Cambria RP, Nienaber CA, et al. STABLE I Investigators. Five-year results from the study of thoracic aortic type B dissection using endoluminal repair (STABLE I) study of endovascular treatment of complicated type B aortic dissection using a composite device design. J Vasc Surg 2019;70:1072-81.e2.
32. Andersen ND, Keenan JE, Ganapathi AM, Gaca JG, McCann RL, Hughes GC. Current management and outcome of chronic type B aortic dissection: results with open and endovascular repair since the advent of thoracic endografting. Ann Cardiothorac Surg 2014;3:264-74.
33. Leshnower BG, Szeto WY, Pochettino A, et al. Thoracic endografting reduces morbidity and remodels the thoracic aorta in DeBakey III aneurysms. Ann Thorac Surg 2013;95:914-21.
34. Conway AM, Qato K, Mondry LR, Stoffels GJ, Giangola G, Carroccio A. Outcomes of thoracic endovascular aortic repair for chronic aortic dissections. J Vasc Surg 2018;67:1345-52.
35. Pellenc Q, Roussel A, De Blic R, et al. False lumen embolization in chronic aortic dissection promotes thoracic aortic remodeling at midterm follow-up. J Vasc Surg 2019;70:710-7.
36. Safi HJ, Estrera AL, Miller CC, et al. Evolution of risk for neurologic deficit after descending and thoracoabdominal aortic repair. Ann Thorac Surg 2005;80:2173-9; discussion 2179.
37. Wahlgren CM, Blohmé L, Günther A, Nilsson L, Olsson C. Outcomes of left heart bypass versus circulatory arrest in elective open surgical descending and thoraco-abdominal aortic repair. Eur J Vasc Endovasc Surg 2017;53:672-8.
39. Hughes GC. Aggressive aortic replacement for Loeys-Dietz syndrome. Tex Heart Inst J 2011;38:663-6.
40. Benrashid E, Wang H, Keenan JE, et al. Evolving practice pattern changes and outcomes in the era of hybrid aortic arch repair. J Vasc Surg 2016;63:323-31.
41. Hughes GC, Vekstein A. Current state of hybrid solutions for aortic arch aneurysms. Ann Cardiothorac Surg 2021;10:731-43.
42. Preventza O, Liao JL, Olive JK, et al. Neurologic complications after the frozen elephant trunk procedure: a meta-analysis of more than 3000 patients. J Thorac Cardiovasc Surg 2020;160:20-33.e4.
43. Benrashid E, Wang H, Andersen ND, Keenan JE, McCann RL, Hughes GC. Complementary roles of open and hybrid approaches to thoracoabdominal aortic aneurysm repair. J Vasc Surg 2016;64:1228-38.
44. Hughes GC, Andersen ND, Hanna JM, McCann RL. Thoracoabdominal aortic aneurysm: hybrid repair outcomes. Ann Cardiothorac Surg 2012;1:311-9.
45. Yang G, Zhang M, Zhang Y, et al. Endovascular repair of postdissection aortic aneurysms using physician-modified endografts. Ann Thorac Surg 2021;112:1201-8.
46. Long CA, Hughes GC. Tech news: physician-modified endografts for endovascular repair of thoracoabdominal aortic aneurysm. Available from: https://www.sts.org/publications/sts-news/tech-news-physician-modified-endografts-endovascular-repair-thoracoabdominal-aortic-aneurysm [Last accessed on 20 Apr 2022].
47. Sandhu HK, Evans JD, Tanaka A, et al. Fluctuations in spinal cord perfusion pressure: a harbinger of delayed paraplegia after thoracoabdominal aortic repair. Semin Thorac Cardiovasc Surg 2017;29:451-9.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Trahanas JM, Jarral OA, Long C, Hughes GC. Management of chronic type B aortic dissection . Vessel Plus 2022;6:49. http://dx.doi.org/10.20517/2574-1209.2021.125
AMA Style
Trahanas JM, Jarral OA, Long C, Hughes GC. Management of chronic type B aortic dissection . Vessel Plus. 2022; 6: 49. http://dx.doi.org/10.20517/2574-1209.2021.125
Chicago/Turabian Style
Trahanas, John M., Omar A. Jarral, Chandler Long, G. Chad Hughes. 2022. "Management of chronic type B aortic dissection " Vessel Plus. 6: 49. http://dx.doi.org/10.20517/2574-1209.2021.125
ACS Style
Trahanas, JM.; Jarral OA.; Long C.; Hughes GC. Management of chronic type B aortic dissection . Vessel Plus. 2022, 6, 49. http://dx.doi.org/10.20517/2574-1209.2021.125
About This Article
Special Issue
Copyright
Data & Comments
Data
 Cite This Article 18 clicks
Cite This Article 18 clicks











Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.