Moderator band connections: an unusual route in retrograde chronic total occlusion procedure: moderator band connections as options to right coronary artery chronic total occlusion
Abstract
We describe a right coronary artery (RCA) chronic total occlusion (CTO) percutaneous coronary intervention (PCI) procedure in a very high risk patient, in whom a complex PCI with the support of Impella CP device plus Rotablator rotational atherectomy was performed 6 months ago to revascularize a very calcified left anterior descendent. This was an unusual approach because it was performed through a very rare connection by retrograde technique. It was performed through a third distal septal branch connecting with the moderator band artery. Reverse controlled antegrade and retrograde tracking technique was then successfully performed. After RCA CTO PCI, there was an improvement in the patient symptoms and quality of life. This case highlights the important role of this unusual and rare source of collateral circulation in RCA CTO.
Keywords
Introduction
The use of the retrograde approach[1-9] has dramatically increased in the last years, not only throug the septal collaterals and saphenous venous graft[10], but also via epicardial connections[11] to the chronic total occlusion (CTO) lesion.
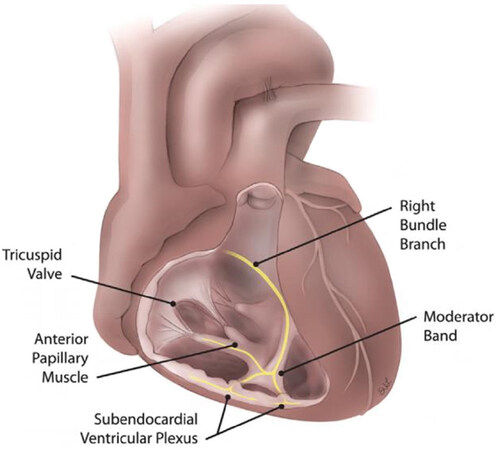
We report the case of a right coronary artery (RCA) CTO recanalized using the retrograde approach through the contralateral channels of a third septal artery connecting with the moderator band artery [Figure 1] that was connected with the right ventricular branch of the RCA.
Case report
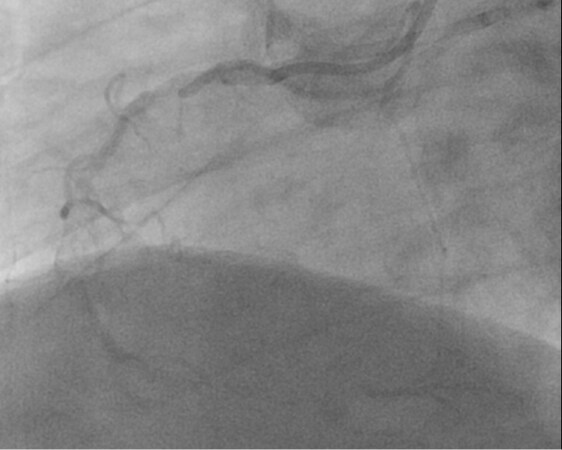
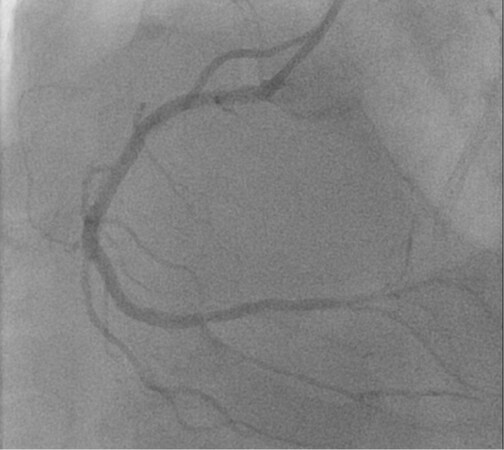
A 64 year-old male, with hypertension, dyslipidemia, left ventricle dysfunction with 35% ejection fraction, and known coronary artery disease. A previous percutaneous coronary intervention (PCI) was performed 6 months before revascularizing an extremely calcified left anterior descendent artery with rotational atherectomy and Impella CP mechanical circulatory support. The patient remained symptomatic due to RCA CTO [Figure 2] with 24% ischemic burden involving the inferior wall in myocardial scintigraphy. Therefore, PCI of RCA CTO was indicated.
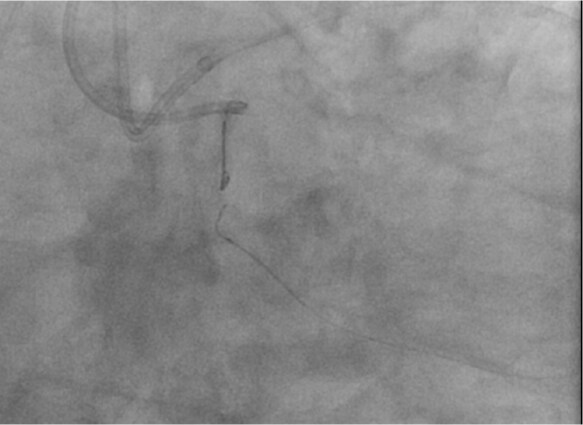
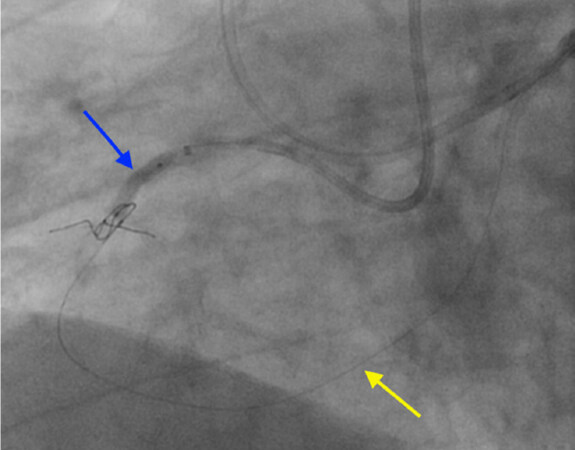
We started the procedure through double femoral access, trying to perform the anterograde approach. We tried to reach the intimal plaque and then the distal vessel, first using AL-1 guide catheter 7F in the RCA, Turnpike spiral microcatheter (Teleflex), Fielder FC guidewire (Asahi Intec.) and Conquest Pro 12 (Asahi Intec.), however without success. After 15 min, we decided to switch retrograde approach, using EBU 4.0 7F guide catheter in left coronary. We used a Turnpike spiral microcatheter (Teleflex) and a Whisper Light Support (Abbott) guidewire to access the third septal, where we could navigate into a connection through the moderator band artery into the right posterior atrioventricular branch. Then, we used the Turnpike Spiral microcatheter to replace the previous guidewire for a new Sion (Asahi Intec.) guidewire due to the fragility of this channel. After accessing the RCA [Figure 3], the reverse controlled antegrade and retrograde tracking technique [Figure 4] was performed and the retrograde guidewire was externalized [RG3 (Asahi Intec.)]. As we reached the RCA in the middle part of the vessel, we used a double lumen catheter TwinPass (Teleflex) to introduce a Fielder FC guidewire anterogradely into the distal RCA, and then PCI with 3 DES Xience Alpine (Abbott) was performed with a good result [Figure 5].
Figure 3. With a Whisper LS we crossed through the moderator band artery to a Right Ventricular Ramus reaching the RCA. RCA: right coronary artery
Figure 4. The yellow arrow shows the route through the moderator band and the blue arrow shows the reverse cart in the proximal RCA. RCA: right coronary artery
Discussion
The retrograde approach has dramatically increased as an alternative to recanalize complex CTO in case of anterograde failure. Data from the ERCTO registry showed that retrograde approach was only used in 15% of the CTO procedures[12]. The septal collaterals are the safest and easiest to track to achieve retrograde access, but in our case we showed an unusual route of the septal channel that was connected probably with the moderator band artery[13]. Sadek et al.[14] described this forgotten access, showing that first, the moderator band is a muscle column that courses inferiorly from the right portion of the interventricular septum to the base of the anterior papillary muscle of the right ventricle. Second, the source of the moderator band artery lies in the first three septal arteries, most often in the second one; in our case we used the less common third one. Finally, this artery makes connections with various branches of the RCA, hence representing a real source of collateral circulation to RCA CTO as we practically demonstrated through this case.
To the best of our knowledge, this is the first case report of a retrograde approach using the moderator band artery as source of collaterals to open a RCA CTO.
In conclusion, the retrograde route described above could be useful for CTO RCA cases after antegrade failure and when standard approach of using the septal collaterals to connect with the posterior descendent artery is not available.
Declarations
Authors’ contributionsContributed substantially in data interpretation and writing: Dallan LAP, Ribeiro MH, Boukhris M
Contributed substantially reviewing the manuscript for important intellectual content: da Silveira JAB, Campos CM, Galassi AR
Contributed substantially in the analysis and interpretation of data: Weilenmann D, da Silveira JAB
Contributed in data collection, interpretation and manuscript review for important intellectual content: Sumitsuji S
Availability of data and materialsNot applicable.
Financial support and sponsorshipNone.
Conflicts of interestAll authors declared that there are no conflicts of interests.
Ethical approval and consent to participateNot applicable.
Consent for publicationNot applicable.
Copyright© The Author(s) 2019.
REFERENCES
1. Sukiennik A, Kasprzak M, Mazurek W, Niezgoda P, Bednarczyk Ł, et al. High-risk percutaneous coronary intervention with Impella CP hemodynamic support. A case series and method presentation. Postepy Kardiol Interwencyjnej 2017;13:67-71.
2. Dudek D, Rakowski T, Sukiennik A, Hawranek M, Dziewierz A, et al. Circulatory support with Impella CP device during high-risk percutaneous coronary interventions: initial experience in Poland. Postepy Kardiol Interwencyjnej 2016;12:254-7.
3. Redondo Dieguez A, Cid Alvarez AB, Trillo Nouche R, López Otero D, Ocaranza Sánchez R, et al. Impella CP-Assisted High-risk Coronary Percutaneous Intervention: First Experience in Spain. Rev Esp Cardiol (Engl Ed) 2017;70:403-5. (in English, Spanish)
4. Kim MH, Kim HJ, Kim NN, Yoon HS, Ahn SH, et al. A rotational ablation tool for calcified atherosclerotic plaque removal. Biomed Microdevices 2011;13:963-71.
5. Marchant E, Martinez A, Fajuri A, Guarda E, Valenzuela E, et al. Rotational atherectomy (Rotablator) for percutaneous transluminal coronary angioplasty. Rev Med Chil 1997;125:1474-82.
6. Dash D. Retrograde coronary chronic total occlusion intervention. Curr Cardiol Rev 2015;11:291-8.
7. Galassi AR, Sianos G, Werner GS, Escaned J, Tomasello SD, et al. Retrograde recanalization of chronic total occlusions in Europe: procedural, in-hospital, and long-term outcomes from the multicenter ERCTO registry. J Am Coll Cardiol 2015;65:2388-400.
8. Reig J, Alberti N, Petit M. Arterial vascularization of the human moderator band: an analysis of this structure's role as a collateral circulation route. Clin Anat 2000;13:244-50.
9. Applegate RJ. Retrograde percutaneous coronary intervention for chronic total occlusion: going backward to go forward. J Am Coll Cardiol 2015;65:2401-3.
10. Nguyen-Trong PK, Alaswad K, Karmpaliotis D, Lombardi W, Grantham JA, et al. Use of saphenous vein bypass grafts for retrograde recanalization of coronary chronic total occlusions: insights from a multicenter registry. J Invasive Cardiol 2016;28:218-24.
11. Benincasa S, Azzalini L, Carlino M, Bellini B, Giannini F, et al. Outcomes of the retrograde approach through epicardial versus non-epicardial collaterals in chronic total occlusion percutaneous coronary intervention. Cardiovasc Revasc Med 2017;18:393-8.
12. Galassi AR, Tomasello SD, Reifart N, Werner GS, Sianos G, et al. In-hospital outcomes of percutaneous coronary intervention in patients with chronic total occlusion: insights from the ERCTO (European Registry of Chronic Total Occlusion) registry. EuroIntervention 2011;7:472-9.
13. Barlis P, Di Mario C. Retrograde approach to recanalising coronary chronic total occlusions immediately following a failed conventional attempt. Int J Cardiol 2009;133:e14-7.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Ribeiro MH, Dallan LAP, da Silva EER, Campos CM, Boukhris M, Galassi AR, Weilenmann D, da Silveira JAB, Sumitsuji S. Moderator band connections: an unusual route in retrograde chronic total occlusion procedure: moderator band connections as options to right coronary artery chronic total occlusion. Vessel Plus 2019;3:21. http://dx.doi.org/10.20517/2574-1209.2018.66
AMA Style
Ribeiro MH, Dallan LAP, da Silva EER, Campos CM, Boukhris M, Galassi AR, Weilenmann D, da Silveira JAB, Sumitsuji S. Moderator band connections: an unusual route in retrograde chronic total occlusion procedure: moderator band connections as options to right coronary artery chronic total occlusion. Vessel Plus. 2019; 3: 21. http://dx.doi.org/10.20517/2574-1209.2018.66
Chicago/Turabian Style
Ribeiro, Marcelo H., Luis A. P. Dallan, Expedito E. Ribeiro da Silva, Carlos M. Campos, Marouane Boukhris, Alfredo R. Galassi, Daniel Weilenmann, João Antônio Brum da Silveira, Satoru Sumitsuji. 2019. "Moderator band connections: an unusual route in retrograde chronic total occlusion procedure: moderator band connections as options to right coronary artery chronic total occlusion" Vessel Plus. 3: 21. http://dx.doi.org/10.20517/2574-1209.2018.66
ACS Style
Ribeiro, MH.; Dallan LAP.; da Silva EER.; Campos CM.; Boukhris M.; Galassi AR.; Weilenmann D.; da Silveira JAB.; Sumitsuji S. Moderator band connections: an unusual route in retrograde chronic total occlusion procedure: moderator band connections as options to right coronary artery chronic total occlusion. Vessel Plus. 2019, 3, 21. http://dx.doi.org/10.20517/2574-1209.2018.66
About This Article
Copyright
Data & Comments
Data

 Cite This Article 0 clicks
Cite This Article 0 clicks










Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.