Research into biodegradable polymeric stents: a review of experimental and modelling work
Abstract
Bioresorbable stents (BRSs) are regarded as the next-generation medical devices to treat blocked or diseased arteries. The use of BRSs aims to reduce the risk of late stent thrombosis and long-term tissue inflammation associated with permanent metallic stents. BRSs are designed to relieve symptoms immediately and also provide mechanical support for an appropriate time period before they are fully absorbed by human body. To promote clinical adoption of BRSs or even to substitute metallic stents, the mechanical performance of BRSs needs to be thoroughly investigated and quantitatively characterised, especially over the full period of degradation. This paper offers a review of current research status of polymeric BRSs, covering both experimental and modelling work. Review of experimental studies highlighted the effects of stent designs and materials on the behaviour of polymeric BRSs. Computational work was able to simulate crimping, expansion and degradation of polymeric BRSs and the results were useful for performance assessment. In summary, the development of polymeric BRSs is still at an early stage, and further research is urgently required for a better understanding and control of their mechanical performance.
Keywords
Introduction
Since the implantation of the first coronary artery stent in 1986, stent deployment has become a standard medical procedure to treat coronary stenosis, a leading cause of heart attack. The worldwide coronary stent market is worth over $7 billion and forecasted to grow by more than 5% annually[1]. Over the past three decades, there have been significant improvements made in stent materials and designs, especially for the drug-eluting stents (DESs) which were firstly approved by Food and Drug Administration (FDA) of USA in 2002. DESs are coated with non-degradable polymer embedded with anti-proliferative drugs, to avoid the occurrence of in-stent restenosis (ISR) which represents a major drawback of bare metal stents (BMSs)[2]. Although the use of DESs can substantially reduce the ISR rates, especially in high-risk patients (lowered by 74%), other clinical problems arise, particularly the increase of late stent thrombosis (ST, with a mortality rate of about 45%) after implantation of DESs[3,4]. The development of deadly ST is concertedly facilitated by hypersensitivity to the permanent presence of alloy and by incomplete repair of the endothelium at the site of vascular wall injury due to the anti-proliferative drug coatings[5]. Also, the presence of permanent stent could cause the increasing risk of strut fracture and failure under complicated loading and corrosive conditions, leading to heart attack or failure, unstable angina and other clinical complications in patients[6].
To overcome these issues, it becomes mandatory to develop next-generation bioresorbable stents (BRSs) to replace metallic ones. Biodegradable polymers have attracted the most interests for manufacturing BRSs[7-9]. Fully expandable biodegradable polymeric stents provide the mechanical support to the vessel wall with appropriate radial strength, to prevent mechanical recoil after immediate implantation. When arterial remodelling achieves a relatively stable phase at 6 months, the mechanical support is no more required. As a result, stents are supposed to be designed to dissolve after 6 months in human body, leaving behind the intact vessel with no pro-inflammatory substances or obstacles[10]. During the process, the biodegradable polymers gradually soften, thus allowing a smooth transfer of the load from the stent to the healing artery, and eventually removing the significantly high stresses induced to the stented artery.
Earlier development of polymeric BRSs includes the Igaki-Tamai stent (Kyoto Medical Planning Co. Ltd, Japan), the Abbott BVS vascular drug-eluting stent (Abbott Vascular, Santa Clara, California, USA) and the REVA stent (Reva Medical, San Diego, California, USA)[8,9]. The Igaki-Tamai stent, made of poly-L-lactic acid (PLLA), has a zig-zag design with straight connective struts. It was the first fully biodegradable polymeric stent ever implanted in humans, and degraded over 18 to 24 months with good performance[8]. The Abbott BVS stent has a bioresorbable polymer backbone of PLLA, incorporated with a polymer coating of poly-DL-lactic acid (PDLLA) containing and controlling the release of the anti-proliferative drug. The BVS 1.0 has out-of-phase sinusoidal rings connected either directly or by straight bridging struts. The first in-man study of BVS 1.0 stents not only highlighted the efficacy and safety of using a biodegradable scaffold, but also provided vital data that help develop the BVS 1.1 stent which has in-phase sinusoidal rings connected by straight bridging struts, which can provide radial support for a longer period of time[9]. This is also the case for REVA stent, which is made of absorbable tyrosine-derived polycarbonate polymer and has a distinctive slide-and-lock design. The preclinical trials of REVA stents have led to the development of the second-generation REZOLVE bioresorbable stent with a helical design[9].
Development of next-generation polymeric BRSs still faces many challenges and unsolved issues, such as stent material and design, mechanical support, in vivo performance, biodegradation rate and manufacturing process. One of the major uncertainties for polymeric BRSs is the effective control of mechanical properties during the biodegradation process. It is very important for BRSs to relieve symptoms immediately and also offer mechanical support for an appropriate period of times. Currently, there is a critical shortage of such data and information, severely limiting the application and further development of BRSs. Designers must use a trial-and-error approach to work out the appropriate material formulation and geometrical parameters of BRSs that can sustain mechanical loads during the degradation process. As an evidence, the concept of a biodegradable polymeric stent dates back to the 1980s, yet currently there are no designs with the FDA approval on the market. Abbott BVS PLLA stent, also named as ABSORB, is a first-of-its-kind device used initially in Europe and parts of Asia Pacific and Latin America to treat arteries with mild restenosis. To promote clinical application at a large scale or even to replace metallic stents, the mechanical performance of BRSs needs to be thoroughly investigated and quantitatively characterised, especially over the full period of degradation. This paper offers a review of current research status of biodegradable polymeric scaffolds, covering both experimental and modelling work.
Experimental studies of BRSs
Mechanical behaviour
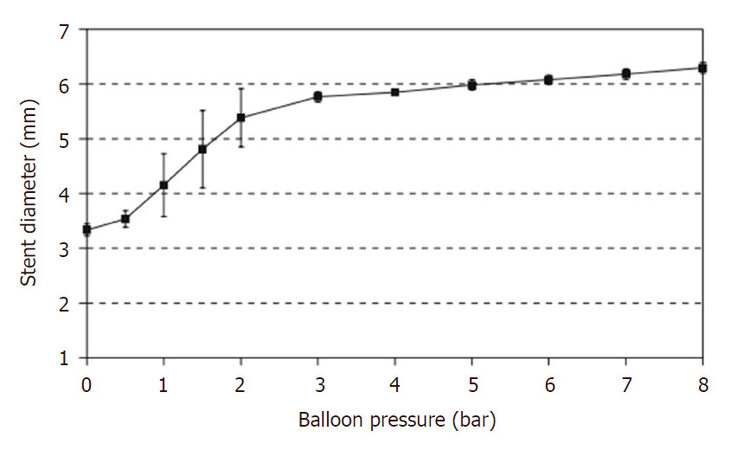
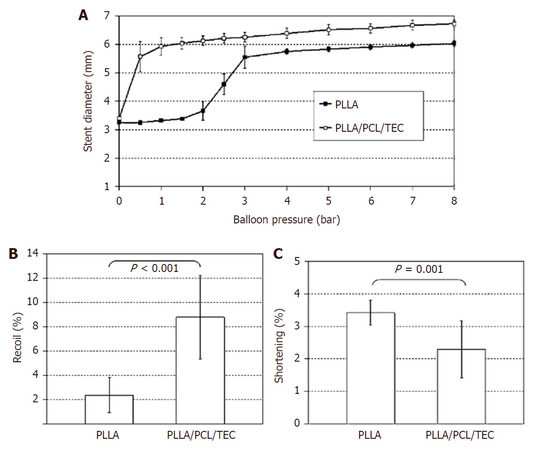
Stents, as medical devices used in human bodies, impose difficulties and challenges for experimental studies due to their tiny size and complex design. Despite the challenges, various methods have already been developed to investigate the behaviour of stents, including polymeric stents. Grabow et al.[11] studied the expansion behaviour of a biodegradable slotted tube stent, made of PLLA and poly-hydroxybutyric acid (PHB), by stent bench testing. As shown in Figure 1, the crimped stent was mounted on a balloon catheter, and then expanded by balloon inflation. All stents were expanded successfully without the occurrence of strut fracture, and Figure 2 shows the stent diameter change as a function of balloon pressure. The stent initially expanded rapidly at a balloon pressure of 1-2 bars and then achieved full expansion at a pressure of 6 bars. The measured recoil effect and collapse pressure were 4.2% and 1.1 bars, respectively. These results revealed that the PLLA/PHB slotted tube stent exhibited adequate mechanical properties during rapid expansion process. The same method was also used by Grabow et al.[12] to investigate the mechanical performance of two types of biodegradable balloon-expandable stents, made of PLLA and PLLA/PCL/TEC, respectively. Both types of stents were able to expand fully by balloon inflation under a pressure of 8 bars, but differences were observed for expansion process as shown in Figure 3. Specifically, the PLLA/polycaprolactone (PCL)/TEC stent expanded immediately with the balloon inflation while the pure PLLA stent started to expand at a balloon pressure of ~2 bars. As a result, the pure PLLA stent achieved a smaller diameter (6.0 mm) than that of PLLA/PCL/TEC stent (6.7 mm) at peak balloon pressure. Moreover, the pure PLLA stent exhibited smaller elastic recoil (2.4%) and larger shortening (3.4%) compared to PLLA/PCL/TEC stent (8.8% and 2.3%, respectively). These results suggested that material properties affected the mechanical behaviour of stents.
Figure 1. Stent in crimped and deployed configurations[11]
Figure 2. Stent diameter change against balloon pressure during expansion[11]
Figure 3. Stent diameter change against balloon pressure (A), elastic recoil (B) and stent shortening (C)[12]
Schmidt et al.[13] characterized the in vitro mechanical performance of bioresorbable scaffolds (i.e., Absorb GT1, Elixir DESlove and Biotronik Dreams 2G) using the same method as described above. The crimped stent had an outer diameter of 1.38 mm, 1.39 mm and 1.44 mm for Absorb GT1, Elixir DESlove and Dreams 2G, respectively. The Dreams 2G exhibited a pushability of 45.41% compared to 33.77% for Absorb GT1 and 36.27% for Elixir DESolve, but no significant difference was found for trackability of the three stents which were 0.68 N, 0.75 N and 0.64 N for Dreams 2G, Absorb GT1 and Elixir DESlove stents, respectively. Moreover, they examined and compared expansion behaviour of the three stents within a mock vessel and a rigid vessel model. The Dreams 2G showed smaller recoil (5.6% and 5.0%) in both two cases without change over time, while Absorb GT1 and Elixir DESolve stents showed time-dependent recoil. These results highlighted the differences between metallic and polymeric BRSs due to different material properties and designs. Ormiston et al.[14] performed expansion and post-dilatation experiments for two commercially available bioresorbable stents (Absorb and DESolve) and compared to typical metallic DES Xience Xpedition. They examined the mechanical characteristics, such as crossing profile, recoil and radial strength, by imaging and intravascular ultrasound techniques. The crossing profile had a diameter of 1.14 mm, 1.43 mm and 1.44 mm for Xpedition, Absorb and DESolve, respectively. The radial strength of stent, measured in terms of pressure required to reduce 25% of cross-sectional area, was found to be 1.6 atm for Xpedition, 1.4 atm for Absorb and 1.1 atm for DESolve. All three stents showed elastic recoil after expansion with a slight change over time. Initially, all three stents significantly recoiled by approximately 0.1 mm. Afterwards, Absorb and Xpedition continued slight recoiling whereas the diameter of DESolve showed an increase (self-correction). Their results revealed that the metallic stent had thinner strut with smaller profile but greater radial strength compared to polymeric stents. Welch et al.[15] studied the effect of thermal annealing on the mechanical behaviour of helical coiled PLLA stents. The stents were annealed at a temperature of 70 °C, 80 °C and 90 °C for 25 min after manufacturing, and then expanded by balloon catheter up to a pressure of 12 atm. Experimental results showed that the stent had higher stiffness and greater collapse resistance with the increase of annealing temperature, whereas the elastic recoil had a decrease. Probably, thermal annealing induced some changes in crystalline structure of PLLA, and thus affected the stress-strain behaviour and stent expansion behaviour.
The experimental work mainly studied the expansion behaviour of polymeric stents, such as stent diameter change against inflation pressure, recoil and shortening effect, which are greatly affected by stent materials and designs. Polymeric BRSs, as the latest generation of stent, are mostly made of biodegradable polymer PLLA. It is well known that PLLA has low mechanical strength and poor elongation compared to metal, which limits its application for stents. Consequently, studies have also been performed to investigate and improve the mechanical behaviour of poly-lactic acid (PLA), including blending PLA with ductile biodegradable polymers as discussed above. In order to further improve the performance of BRSs and compete with metallic stents, research into processing and characterisation of biodegradable polymers is particularly required.
Degradation behaviour
One of key features for polymeric stents is their degradation behaviour over time. There were some experimental studies available in terms of characterization of stent degradation in vitro and in vivo. Xu et al.[16] evaluated in vitro and in vivo degradation behaviour of biodegradable tubular stents, made of poly-lactic-co-glycolic acid (PLGA) with five different molar weight ratios of LA/GA (50/50, 60/40, 71/29, 80/20 and 88/12), for application in common bile duct (CBD) repair and reconstruction. For in vitro test, stents were placed in bile degradation medium (pH = 7.2-7.6). Morphological results showed that the stents slightly expanded, deformed and then cracked meanwhile their colour changed from initially transparent to yellow and opaque due to the bile and water absorption. Weight loss, molecular weight change and water uptake were also observed, indicating the PLGA stents exhibited different degradation rates due to different composition ratios. For in vivo test, PLGA (71/29) stents were implanted in the rat CBDs. Results showed that the polymeric stents can provide the same biomedical functions as typical T tubes and completely disappeared after 5 weeks.
Hadaschik et al.[17] investigated the degradation behaviour of a new biodegradable ureteral stent (Uriprene) made of copolymer PLGA (LA/GA = 80/20) using porcine models. Uriprene stents were implanted in 20 pigs while standard biostable stents were implanted in 16 pigs as a control. Compared to control stents, Uriprene stents caused significantly less ureteral dilatation and urinary tract infections. Their results also showed that the Uriprene stents began degradation at week 3, and completely degraded at week 10. The novel stent was proved to be biocompatible in vivo. Yang et al.[18] carried out degradation experiments on a novel biodegradable PGLA ureteral stent, with multilayer design immersed by microsphere zein and BaSO4, in human urine in vitro. The scanning electron microscope (SEM) results showed that the novel stent started degradation at week 2 and fully degraded after 4 weeks, and the degradation happened layer by layer from outer to inner surface. The stent weight and mechanical strength (i.e., tensile strength, elastic recovery and radial compression load) showed a decrease over the degradation time.
Currently, commercial degradable polymeric stents are made of PLLA, which breaks down to natural by-products, i.e., water, gases (CO2 and N2), biomass and inorganic salts. These natural by-products are non-toxic, so there are no negative effects on the blood or vessel wall. Degradation behaviour of polymeric stents was mainly characterized by in vitro and in vivo methods, focusing on variation of physical (e.g., mass weight and molecular weight) and mechanical properties (e.g., tensile strength and elastic modulus) over degradation times. Key parameters used to assess degradation behaviour of biodegradable polymers include mass loss, molecular weight change, water uptake and morphology change. Gong et al.[19] carried out in vitro degradation study of porous PLLA scaffolds over 39 weeks, and the scaffolds degraded at a slow rate due to its highly porous structure in terms of weight water uptake and structure change. As reported by Liu et al.[20], PLLA porous scaffolds exhibited a reduction in mass and molecular weight during an in vitro degradation time of 200 days. Rodrigues et al.[21] studied degradation process of porous PLA scaffold immersed in phosphate-buffered-saline solution, and revealed that there was no significant change in molecular weight over 8 weeks. Zamiri et al.[22] compared the in vitro degradation behaviour of PLLA and PLLA/PLGA braided scaffolds over 25 weeks, and the mass loss was found very limited for PLLA braided scaffolds whereas PLLA/PLGA braided scaffolds experienced a mass loss of 64%. Grabow et al.[12] reported a gradual and steady reduction in molecular weight for a PLLA scaffold prototype during 24 weeks of in vitro degradation. Table 1 gives a summary of these key parameters used in assessing degradation behaviour of polymer scaffolds.
Key parameters used in assessing degradation behaviour of polymer scaffolds
| References | Gong et al.[19] (2007) | Liu et al.[20] (2014) | Rodrigues et al.[21] (2016) | Zamiri et al.[22] (2010) | Grabow et al.[12] (2007) |
|---|---|---|---|---|---|
| Materials | PLLA scaffold | PLLA scaffold | Porous PLA scaffold | PLLA scaffold/PLGA scaffold | PLLA scaffold |
| Media | PBS | PBS | PBS | PBS | PBS |
| Degradation times | 39 weeks | 200 days | 8 weeks | 25 weeks | 24 weeks |
| Mass loss | 30% | 8% | Remain relatively constant | 5%/64% | - |
| Molecular weight loss | From 177,000 to 80,000 | From 179,000 to 146,000 | No significant change (120,000~150,000) | - | 28% |
| Water uptake | Decreased dramatically with degradation time, and lowest value appeared between week 9 and 12 | 900% | - | - | - |
| Morphology change | Microcracks at week 9; more cracks and big holes after week 23 | Some little holes on the surface of the porous walls | - | - | - |
Mechanical properties (i.e., ductility, toughness and strength) of biodegradable polymers change significantly during degradation due to hydrolytic chain scission at molecule level. It is of importance to understand the mechanical behaviour of bioresorbable polymeric scaffolds during degradation period. The earliest assessment of the mechanical performance of biodegradable stents was conducted by Agrawal et al.[23], who tested in vitro the pressure-diameter behaviour of the Duke biodegradable stents made of PLLA fibres. They reported that with a careful balance between fibre mechanical properties (varied with draw ratio and thermal treatments) and stent designs, it was possible to achieve a successful biodegradable stent. Zilberman et al.[24] reported a loss in radial compression strength for their PLLA stent designs with degradation time, which is also associated with reductions in elastic modulus and yield strain of the PLLA fibres. Nuutinen et al.[25] carried out in vitro tests of a woven fibre polymeric braided stent subjected to radial compression in a pressurized chamber. The stent design did not perform well enough when made of biodegradable polymer, and the collapse pressure was still lower than its metal counterpart even with thicker fibres. Specifically, the stent lost structural integrity after 36 weeks of degradation (immersed in saline at 37 °C) and the collapse pressure decreased by half at 30 weeks. The in vitro degradation study by Liu et al.[26] showed that PLLA porous scaffolds exhibited a reduction in compressive modulus and strength during a degradation time of 200 days. Recently, Rodrigues et al.[21] carried out an in vitro degradation study of porous PLA scaffold immersed in phosphate-buffered-saline solution for 8 weeks. The study revealed that compressive properties (i.e., compressive modulus and stress at yield) of the scaffolds maintained constant during the initial 6 weeks and increased significantly at week 8. Similarly, Grabow et al.[12] conducted in vitro degradation study for a PLLA scaffold prototype in a deployed shape, and they found that collapse pressure increased firstly within 12 weeks and then deceased. From the material point of view, the initial increase of compressive properties might be caused by the recrystallization of biodegradable polymer PLA/PLLA due to the water absorption and temperature increase (from room temperature 20 °C to human body temperature 37 °C). It was reported that crystallization can significantly improve the mechanical strength and stiffness of PLLA. It should be pointed out that there is a lack of efforts in assessing the discontinuity of the scaffold during the late stage of degradation, due to the difficulties in imaging the scaffold. However, such studies can be accomplished by using the micro computed tomography (CT) technology to investigate the internal damage associated with both biodegradation and mechanical deformation wherever feasible. Also the microstructures of all specimens can also be investigated using SEM both before and after the tests, by fracturing the specimens (e.g., in liquid nitrogen) and coating the fracture surfaces with a thin layer of gold.
In addition, clinical trials have also been carried out extensively and long-term follow up indicated the safety and efficacy of polymeric stents in treatment of coronary artery disease. Follow-up studies, based on invasive imaging methods such as CT, angiography and intravascular ultrasound (IVUS), were normally carried out to assess the stented vessel after the implantation of bioresorbable scaffolds. As reported in Ormiston et al.[27], the bioresorbable vascular scaffold (BVS) absorb showed an overall 16.8% reduction of lumen area at 6-month follow-up of 30 patients implanted with the scaffolds. Serruys et al.[28] evaluated the outcomes of Absorb for treating coronary artery stenosis in 45 patients. The mean lumen area was found to decrease by 3.1% (6.60 to 6.37 mm2) according to IVUS analysis at 6-month follow up whereas it increased to 6.85 mm2 at 2-year follow up. Recent 5-year follow-up results after Absorb implantation concluded that the mean lumen area tended to increase from 6 months to 1 year and 5 years[29]. Progressive lumen gain was also observed after Absorb implantation in porcine coronary arteries[30], for which the lumen area kept stable up to 6 months and then showed a progressive increase from one to 3.5 years. These studies confirmed the lumen gain after scaffold implantation over the degradation times, especially from 6 months onwards.
However, studies are still limited and challenging due to the microscale geometry of stent and complex environment of human artery. To complement experimental work, finite element simulations were consequently used to study the stent performance during deployment, which is reviewed in the next section.
Computational work
Stent deployment
Finite element (FE) modelling is of particular help in evaluating stent performance. However, most FE modelling of stent implantation, including recent ones, were dealing with metallic stents such as the effects of design and material on stent expansion, recoiling and dogboning[31-33]. FE modelling of polymeric BRSs is very limited, especially how they compare with metallic stents in terms of mechanical performance. There are only a few papers in literature. For instance, Pauck and Reddy[34] simulated the mechanical performance of PLLA stents with different designs and varying polymer stiffness. Material stiffness and geometrical design affects the radial strength of polymeric stent significantly. Debusschere et al.[35] studied the free-expansion behaviour of bioresorbable Absorb stent by considering the viscoplasticity of the material. They simulated stent expansion by increasing inflation pressure linearly or in a stepwise, and linear inflation method was found to induce higher stress concentration in the U-bend struts. Inflation rate affected stent expansion mainly during inflation process, while not much difference was shown after balloon deflation. Wang et al.[36] studied the mechanical deformation of a PLLA biodegradable coronary stent using experimental and computational methods. They modelled the crimping of stent to an outer diameter of 1.41 mm and subsequent expansion to different inner diameters. Stent deformation profiles were in good agreement with experimental ones during both crimping and expansion processes, and large deformation occurred at sharp curvature of struts in all cases. The radial recoil ratio showed a decrease trend with the increase of stent expansion, which was 4.19%, 2.92% and 1.81% obtained for stent with expanding to 3.1 mm, 3.7 mm and 3.92 mm, respectively. They also modelled re-crimping of the expanded stent to evaluate the radial strength and stiffness, and calculated radial strength and stiffness was 1.46 N/mm (close to the experimental value of 1.55 N/mm) and 1.40%, respectively. Shanahan et al.[37] developed a viscoelastic material model for a biodegradable polymeric braided stent, and evaluated the time-dependent viscoelastic behaviour using finite element method. They simulated the crimping of stent by enforcing radial displacement on 8 rigid plates, and the linear viscoelastic material model was validated against their experimental data. However, no significant difference was observed for the crimping behaviour of braided stent modelled as either linear elastic or viscoelastic material. However, all these simulation work neglected the diseased artery in their models and was unable to assess the performance of polymeric stents comprehensively.
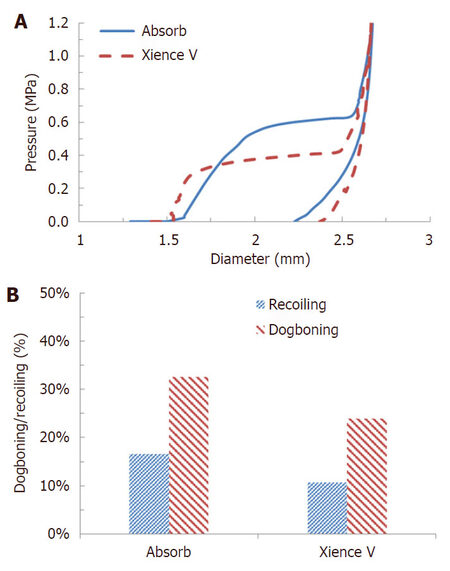
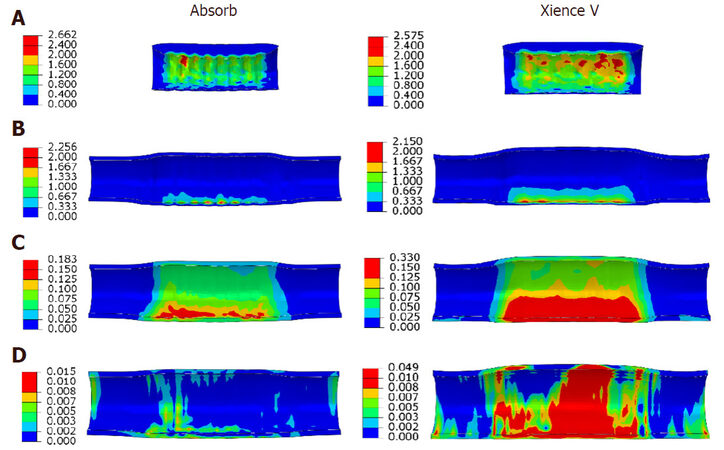
Very recently, Schiavone et al.[38] carried out a comparative study for polymeric Absorb stent and metallic Xience stent by including diseased artery in finite element simulations. The Absorb stent showed a lower rate of expansion in diseased artery, with higher dog-boning and recoiling when compared to Xience stent [Figure 4]. This was due to the difference in material property and stent design. It was suggested that post-dilatation of Absorb stent is required in order to achieve an effective treatment of stenosis, especially for patients with stiffer vessels and highly calcified plaques. However, significantly lower stress was induced to the plaque-artery system treated with the Absorb stent, which is a clinical benefit in terms of causing less injury to the vessels. Effect of plaque eccentricity was also evaluated in their simulations, and higher stress was found for the media and adventitia tissue layers with the increase of plaque eccentricity [Figure 5]. Eccentric plaque also caused complications to stent implantation, such as non-uniform stress distribution and artery expansion. As such, the selection of stents, in terms of designs and materials, will be of high importance for patients in order to achieve the most effective clinical outcomes.
Figure 4. (A) Stent outer diameter change against pressure and (B) recoiling and dogboning effects for Absorb scaffold and Xience V stent in concentric lesion[38]
Figure 5. Contour plot of the maximum principal stress (MPa) on the (A) plaque, (B) intima layer, (C) media layer and (D) adventitia layer, after deployment of Absorb scaffold and Xience V stent in eccentric lesion[38]
Stent degradation
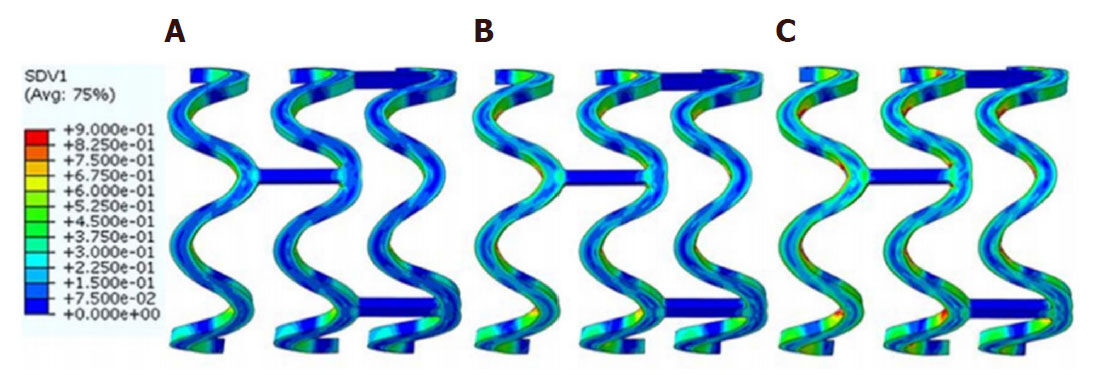
BRSs have advantages in overcoming clinical complications (e.g., restenosis and ST) associated with permanent metallic stents due to their biodegradation characteristics. Generally, constitutive models are required to describe the mechanical response of stent materials during the process of degradation. For instance, Soares et al.[39] applied a thermodynamically consistent constitutive model to predict degradation behaviour of PLLA stents. This model was suitable for simulating deformation-induced degradation, especially for biodegradable PLLA. The model is based on a degradation-dependent Helmholtz potential (material properties decrease as a function of degradation) and the rate of dissipation. Degradation of three different stent designs was modelled, and results showed that high risk of degradation was mainly observed at the bends of stent rings and junction points. Luo et al.[40] developed a numerical model to study the degradation behaviour of bioabsorbable PLLA stent. The constitutive degradation model combined the degree of degradation with pre-stretched deformation, and the degree of degradation was used to describe the change of material property as a function of degradation time. The degradation model was validated against experimental tensile data at different degradation times. Results showed that degradation happened throughout the whole stent over 30 days, but the degradation rate was not uniform [Figure 6]. The maximum degradation was observed at the inner surface of U-bend strut where the stress concentration/maximum strain occurred during stent expansion, which was in good agreement with experimental result. This indicated that the degradation rate of material was influenced by the initial deformation.
Figure 6. Degradation degree distribution on the stent over time[40]. (A) 10 days degradation; (B) 20 days degradation; (C) 30 days degradation
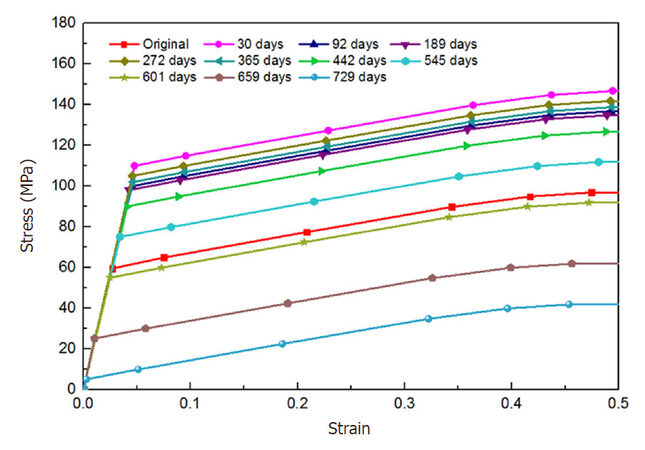
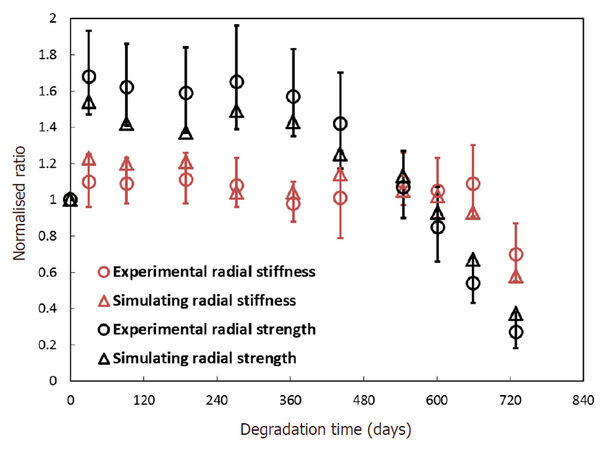
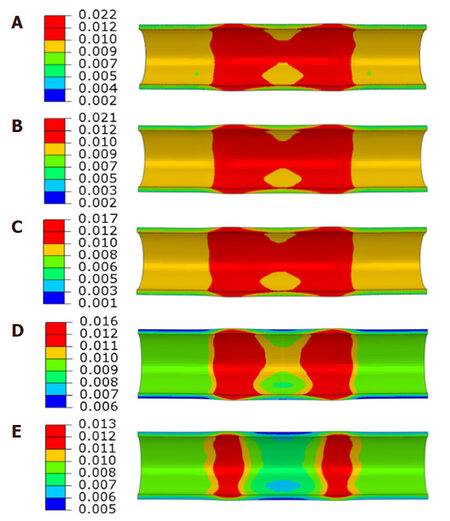
Material property of biodegradable polymer shows a difference during degradation, and therefore mechanical behaviour of polymeric stents is also influenced by stent degradation. Several studies have been carried out to predict the degradation behaviour of polymeric stents by developing constitutive models for degradable material, but neglected stent-artery interaction during degradation. For the first time, Qiu et al.[41] evaluated the mechanical behaviour of a polymeric BRS using computational method, with a focus on stent-artery interaction during the process of degradation and artery remodelling. In particular, stress-strain responses were calibrated for polymeric stents over 2-year in vitro degradation period, according to experimentally measured strength and stiffness [Figures 7 and 8]. Effect of degradation on stent behaviour was simulated by considering the change of material’s property over time. In addition, vessel remodelling was simulated by manually changing the geometry of diseased artery, following those published clinical data. Over 2-year degradation times, stresses in the plaque and vessel layers showed a consistent decrease; while the stent experienced an increase in stress at the beginning followed by a gradual decrease, corresponding to the changing properties of the polymeric material [Figure 9]. In addition, vessel remodelling led to a reduction of stress for the whole scaffold-plaque-artery system. This work offered valuable insights into interactive behaviour between a bioresorbable stent and diseased artery during a 2-year period of in vitro degradation, which is helpful for developing new-generation BRSs for treating artery stenosis.
Figure 7. Constructed poly-L-lactic acid stress-strain curves for Absorb scaffold at different degradation time points[41]
Figure 8. Radial strength and stiffness data obtained from simulation for Absorb scaffold compared to experimental data at different degradation time points[41]
Figure 9. Contour plot of the maximum principal stress on the media layer at a degradation time of 0 day (A), 189 days (B), 365 days (C), 659 days (D) and 729 days (E)[41]
The work of Qiu et al.[41] highlighted that for percutaneous coronary intervention, stent deployment causes severe stresses to the artery, which will induce negative influence such as damage to arterial tissue. Thus, it is of importance to assess the stress state produced in the artery-plaque system during stent implantation process. A desirable process of stent implantation requires an outcome of expansion which is enough to relieve vessel obstruction and also causes least damage to the arterial walls[42], as unsuccessful deployment may trigger ISR. Here, unsuccessful deployment includes injury and excessive stretch of arterial walls, under-expansion of stent and structural failure of struts. A strong correlation between severe wall stresses and high restenosis rate has been confirmed by literature[43]. Clearly, it is also necessary to assess the safety and efficacy of polymeric stents during degradation, especially stent-artery interaction. The work of Qiu et al.[41] is the first attempt to model the mechanical interaction of BRS with stenotic artery over the full process of stent degradation. A general reduction of stresses was shown for the plaque and vessel layers over stent degradation, which can be beneficial for the natural healing of stented artery.
So far, computational work has focused on the development and validation of material constitutive models that can predict the mechanical behaviour of degradable polymer or implant[44,45]. There is not a model available yet to model the degradation process as well as property changes, especially to predict both biodegradable implant mechanics and its interaction with blood vessel. For instance, finite-element models were used to predict the recoil and collapse behaviour of polymer stent design by considering the elastic and/or inelastic behaviour of the polymer[46,47], but neglecting any changes of material properties that occur with degradation[48]. At human-body temperature, the biodegradation process is a combined effect of time and local deformation. To study this process appropriately, it is necessary to couple the visco-deformation model with biodegradation. In this case, a damage tensor needs to be introduced into the model to simulate the material degradation process, linked with the multi-axial stress/strain states in the implanted stent. The evolution of this damage tensor will depend on mechanical deformation and subsequently affect the mechanical properties as a result of material degradation[49]. In this way, the interplay between deformation and degradation can be modelled, including the influence of deformation rate and material composition, which has not been previously reported for biodegradable polymeric stents[44]. This type of model, although not available yet, can best simulate the degradation process and help predict the biological outcome due to progressively changing load-bearing property of vascular implant during degradation process.
Loading rate dependency
It is well known that PLLA has low mechanical strength and poor elongation compared to metal, which limits its application for stents. Based on literature review, a number of experimental studies have been performed to investigate and improve the mechanical behaviour of PLA, including adding plasticizers to PLA and blending PLA with ductile biodegradable polymers. Also, different constitutive material models (e.g., elastic-plastic model and viscoelastic model) were applied to model the deformation of PLLA stent. It should be noted that the stress-strain behaviour of polymers is affected by strain rate, which indicates the time-dependent deformation nature of the materials (an increase of stress level with the increase of loading rate). Consequently, consideration of the time-dependent or viscous behaviour of the materials should be given during the process of designing and manufacturing of polymeric devices, including computational studies.
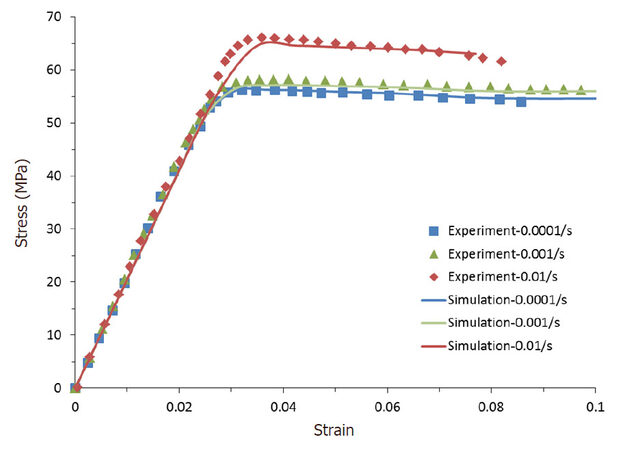
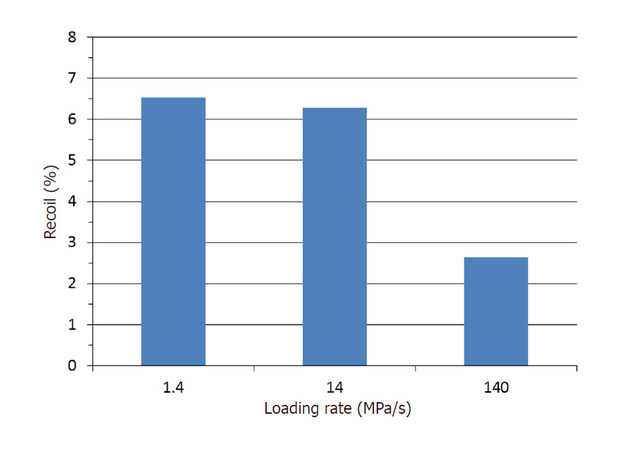
Only recently, Qiu et al.[50] applied an elastic-plastic constitutive model with time dependency to model free expansion of Elixir stent under a loading rate of 1.4, 14 and 140 MPa/s, respectively. Loading-rate dependence was described by inputting the ratio of yield stress as a function of plastic-strain rate. As shown in Figure 10, the rate-dependent stress-strain response of a PLA and poly-butylene-succinate (PBS) copolymer (with a weight ratio of 70% to 30%) was simulated very well by the rate-dependent elastic-plastic model[50]. After expansion, stresses developed in the stent was dependent on the loading rates, for both magnitude and distribution. Stent recoiling showed a significant reduction when the loading rate was changed from 1.4 to 140 MPa/s, as shown in Figure 11. These results proved that polymeric stent behaved differently during expansion process if the loading rate was different. With the increase of inflating rate, stent intended to expand further, with reduced recoiling but higher level of stresses. These results suggest that loading rate should be taken as an additional factor in the surgical practice of stent deployment.
Figure 10. Experimental and simulated stress-strain behaviours of blended PLA/PBS (70/30) for different strain rates[50]
Figure 11. Recoiling effect of the Elixir stent for different loading rates[50]
Conclusions
Stents have been developed from BMSs, to DESs and then BRSs to prevent various complications and improve their clinical efficacy. Materials are also extended from metal (e.g., stainless steel and cobalt-chromium alloy) to biodegradable polymer (PLLA). For polymeric stents, experimental studies showed stent designs and materials played an important role in the stent behaviour during expansion. Physical properties (e.g., mass weight and molecular weight) and mechanical properties (e.g., tensile strength and elastic modulus) showed a difference during stent degradation. Computational approaches have also been used to study the stent performance during expansion and degradation. However, the development of bioresorbable polymeric stents is still ongoing, and studies are extremely limited due to the microscale geometry of stent and complex environment of human artery. Therefore, further research is urgently required for a better understanding of the mechanical performance of polymeric stents, including long term clinical outcomes.
Declarations
Authors’ contributionsCarried out the review and drafted the paper: Qiu T
Discussed about the technical contents and also contributed to the writing of the review paper: Zhao L
Availability of data and materialsNot applicable.
Financial support and sponsorshipNone.
Conflicts of interestAll authors declared that there are no conflicts of interest.
Ethical approval and consent to participateNot applicable.
Consent for publicationNot applicable.
Copyright© The Author(s) 2018.
REFERENCES
1. Moore JE Jr, Soares JS, Rajagopal KR. Biodegradable stents: biomechanical modelling challenges and opportunities. Cardiovasc Eng Technol 2010;1:52-65.
2. Hoffmann R, Mintz GS. Coronary in-stent restenosis - predictors, treatment and prevention. Eur Heart J 2000;21:1739-49.
3. Pfisterer ME. Late stent thrombosis after drug-eluting stent implantation for acute myocardial infarction: a new red flag is raised. Circulation 2008;118:1117-9.
4. Iakovou I, Schmidt T, Bonizzoni E, Ge L, Sangiorgi GM, Stankovic G. Incidence, predictors, and outcome of thrombosis after successful implantation of drug-eluting stents. J Am Med Assoc 2005;293:2126-30.
5. Joner M, Finn AV, Farb A, Mont EK, Kolodgie FD, Ladich E, Kutys R, Skorija K, Gold HK, Virmani R. Pathology of drug-eluting stents in humans: delayed healing and late thrombotic risk. J Am Coll Cardiol 2006;48:193-202.
6. Yang TH, Kim DI, Park SG, Seo JS, Cho HJ, Seol SH, Kim SM, Kim DK, Kim DS. Clinical characteristics of stent fracture after sirolimus- eluting stent implantation. Int J Cardiol 2009;131:212-6.
7. Flege C, Vogt F, Höges S, Jauer L, Borinski M, Schulte VA, Hoffmann R, Poprawe R, Meiners W, Jobmann M, Wissenbach K, Blindt R. Development and characterization of a coronary polylactic acid stent prototype generated by selective laser melting. J Mater Sci Mater Med 2013;24:241-55.
9. Onuma Y, Serruys PW. Bioresorbable scaffold: the advent of a new era in percutaneous coronary and peripheral revascularization? Circulation 2011;123:779-97.
10. Waksman R. Biodegradable stents: they do their job and disappear. J Invasive Cardiol 2006;18:70-4.
11. Grabow N, Bünger CM, Schultze C, Schmohl K, Martin DP, Williams SF, Sternberg K, Schmitz KP. A biodegradable slotted tube stent based on poly (L-lactide) and poly (4-hydroxybutyrate) for rapid balloon-expansion. Ann Biomed Eng 2007;35:2031-8.
12. Grabow N, Bünger CM, Sternberg K, Mews S, Schmohl K, Schmitz KP. Mechanical properties of a biodegradable balloon-expandable stent from poly (L-lactide) for peripheral vascular applications. J Med Devices 2007;1:84-8.
13. Schmidt W, Behrens P, Brandt-Wunderlich C, Siewert S, Grabow N, Schmitz KP. In vitro performance investigation of bioresorbable scaffolds-standard tests for vascular stents and beyond. Cardiovasc Revasc Med 2016;17:375-83.
14. Ormiston JA, Webber B, Ubod B, Darremont O, Webster MW. An independent bench comparison of two bioresorbable drug-eluting coronary scaffolds (Absorb and DESolve) with a durable metallic drug-eluting stent (ML8/Xpedition). EuroIntervention 2015;11:60-7.
15. Welch TR, Eberhart RC, Reisch J, Chuong CJ. Influence of thermal annealing on the mechanical properties of PLLA coiled stents. Cardiovasc Eng Technol 2014;5:270-80.
16. Xu X, Liu T, Zhang K, Liu S, Shen Z, Li Y, Jing X. Biodegradation of poly (l-lactide-co-glycolide) tube stents in bile. Polym Degrad Stab 2008;93:811-7.
17. Hadaschik BA, Paterson RF, Fazli L, Clinkscales KW, Shalaby SW, Chew BH. Investigation of a novel degradable ureteral stent in a porcine model. J Urol 2008;180:1161-6.
18. Yang G, Xie H, Huang Y, Lv Y, Zhang M, Shang Y, Zhou J, Wang L, Wang JY, Chen F. Immersed multilayer biodegradable ureteral stent with reformed biodegradation: an in vitro experiment. J Biomater Polym 2017;31:1235-44.
19. Gong Y, Zhou Q, Gao C, Shen J. In vitro and in vivo degradability and cytocompatibility of poly (l-lactic acid) scaffold fabricated by a gelatin particle leaching method. Acta Biomaterials 2007;3:531-40.
20. Liu YS, Huang QL, Kienzle A, Müller WEG, Feng QL. In vitro degradation of porous PLLA/pearl powder composite scaffolds. Mater Sci Eng C 2014;38:227-34.
21. Rodrigues N, Benning M, Ferreira AM, Dixon L, Dalgarno K. Manufacture and characterisation of porous PLA scaffolds. Procedia CIRP 2016;49:33-8.
22. Zamiri P, Kuang Y, Sharma U, Ng TF, Busold RH, Rago AP, Core LA, Palasis M. The biocompatibility of rapidly degrading polymeric stents in porcine carotid arteries. Biomaterials 2010;31:7847-55.
23. Agrawal CM, Haas KF, Leopold DA, Clark HG. Evaluation of poly(L-lactic acid) as a material for intravascular polymeric stents. Biomaterials 1992;13:176-82.
24. Zilberman M, Nelson KD, Eberhart RC. Mechanical properties and in vitro degradation of bioresorbable fibers and expandable fiber-based stents. J Biomed Mater Res B 2005;74:792-9.
25. Nuutinen JP, Clerc C, Reinikainen R, Törmälä P. Mechanical properties and in vitro degradation of bioabsorbable self-expanding braided stents. J Biomate Sci 2003;14:255-66.
26. Liu G, Zhang X, Wang D. Tailoring crystallization: towards high-performance poly (lactic acid). Adv Mater 2014;26:6905-11.
27. Ormiston JA, Serruys PW, Regar E, Dudek D, Thuesen L, Webster MW, Onuma Y, Garcia-Garcia HM, McGreevy R, Veldhof S. A bioabsorbable everolimus-eluting coronary stent system for patients with single de-novo coronary artery lesions (ABSORB): a prospective open-label trial. Lancet 2008;371:899-907.
28. Serruys PW, Onuma Y, Ormiston JA, de Bruyne B, Regar E, Dudek D, Thuesen L, Smits PC, Chevalier B, McClean D, Koolen J. Evaluation of the second generation of a bioresorbable everolimus drug-eluting vascular scaffold for treatment of de novo coronary artery stenosis clinical perspective. Circulation 2010;122:2301-12.
29. Serruys PW, Ormiston J, van Geuns RJ, de Bruyne B, Dudek D, Christiansen E, Chevalier B, Smits P, McClean D, Koolen J, Windecker S. A polylactide bioresorbable scaffold eluting everolimus for treatment of coronary stenosis. J Ame Col Cardio 2016;67:766-76.
30. Lane JP, Perkins LE, Sheehy AJ, Pacheco EJ, Frie MP, Lambert BJ, Rapoza RJ, Virmani R. Lumen gain and restoration of pulsatility after implantation of a bioresorbable vascular scaffold in porcine coronary arteries. Cardiovas Interven 2014;7:688-95.
31. Chua SD, Mac Donald BJ, Hashmi MSJ. Finite element simulation of stent and balloon interaction. J Mater Pro Tech 2003;143:591-7.
32. Lally C, Dolan F, Prendergast PJ. Cardiovascular stent design and vessel stresses: a nite element analysis. J Biomech 2005;38:1574-81.
33. Schiavone A, Zhao LG, Abdel-Wahab AA. Effects of material, coating, design and plaque composition on stent deployment inside a stenotic artery -- nite element simulation. Mater Sci Eng C Mater Biol Appl 2014;42:479-88.
34. Pauck RG, Reddy BD. Computational analysis of the radial mechanical performance of PLLA coronary artery stents. Med Eng Phys 2015;37:7-12.
35. Debusschere N, Segers P, Dubruel P, Verhegghe B, De Beule M. A finite element strategy to investigate the free expansion behaviour of a biodegradable polymeric stent. J Biomech 2015;48:2012-8.
36. Wang Q, Fang G, Zhao Y, Wang G, Cai T. Computational and experimental investigation into mechanical performances of poly-L-lactide acid (PLLA) coronary stents. J Mech Behav Biomed Mater 2017;65:415-27.
37. Shanahan C, Tofail SA, Tiernan P. Viscoelastic braided stent: finite element modelling and validation of crimping behaviour. Mater Design 2017;121:143-53.
38. Schiavone A, Abunassar C, Hossainy S, Zhao LG. Computational analysis of mechanical stress-strain interaction of a bioresorbable scaffold with blood vessel. J Biomech 2016;49:2677-83.
39. Soares JS, Moore JE, Rajagopal KR. Modeling of deformation-accelerated breakdown of polylactic acid biodegradable stents. J Med Devices 2010;4:410-7.
40. Luo Q, Liu X, Li Z, Huang C, Zhang W, Meng J, Chang Z, Hua Z. Degradation model of bioabsorbable cardiovascular stents. PLoS One 2014;9:e110278.
41. Qiu T, He R, Abunassar C, Hossainy S, Zhao LG. Effect of two-year degradation on mechanical interaction between a bioresorbable scaffold and blood vessel. J Mech Behav Biomed Mater 2017;78:254.
42. Farooq V, Gogas BD, Serruys PW. Restenosis delineating the numerous causes of drug-eluting stent restenosis. Circ Cardiovasc Interv 2010;4:195-205.
43. Imani SM, Goudarzi AM, Ghasemi SE, Kalani A, Mahdinejad J. Analysis of the stent expansion in a stenosed artery using finite element method: application to stent versus stent study. Proc Inst Mech Eng H 2014;228:996-1004.
44. Soares JS, Moore JE Jr, Rajagopal KR. Constitutive framework for biodegradable polymers with applications to biodegradable stents. Asaio 2008;54:295-301.
45. Vieira AC, Vieira JC, Ferra JM, Magalhães FD, Guedes RM, Marques AT. Mechanical study of PLA-PCL fibers during in vitro degradation. J Mechan Behar Biomed Mater 2011;4:451-60.
46. Grabow N, Bünger CM, Schultze C, Schmohl K, Martin DP, Williams SF, Sternberg K, Schmitz KP. A biodegradable slotted tube stent based on poly(L-lactide) and poly(4-hydroxybutyrate) for rapid balloon-expansion. Ann Biomed Eng 2007;35:2031-8.
47. Grabow N, Schlun M, Sternberg K, Hakansson N, Kramer S, Schmitz KP. Mechanical properties of laser cut poly(L-lactide) micro-specimens: implications for stent design, manufacture, and sterilization. ASME J Biomechan Eng 2008;127:25-31.
48. Moore JE Jr, Soares JS, Rajagopal KR. Biodegradable stents: biomechanical modeling challenges and opportunities. Cardiovas Eng Tech 2015;1:52-65.
49. Wu W. Experimental data confirm numerical modeling of the degradation process of magnesium alloys stents. Acta Biomateralia 2013;9:8730-9.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Qiu T, Zhao L. Research into biodegradable polymeric stents: a review of experimental and modelling work. Vessel Plus 2018;2:12. http://dx.doi.org/10.20517/2574-1209.2018.13
AMA Style
Qiu T, Zhao L. Research into biodegradable polymeric stents: a review of experimental and modelling work. Vessel Plus. 2018; 2: 12. http://dx.doi.org/10.20517/2574-1209.2018.13
Chicago/Turabian Style
Qiu, Tianyang, Liguo Zhao. 2018. "Research into biodegradable polymeric stents: a review of experimental and modelling work" Vessel Plus. 2: 12. http://dx.doi.org/10.20517/2574-1209.2018.13
ACS Style
Qiu, T.; Zhao L. Research into biodegradable polymeric stents: a review of experimental and modelling work. Vessel Plus. 2018, 2, 12. http://dx.doi.org/10.20517/2574-1209.2018.13
About This Article
Copyright
Data & Comments
Data
 Cite This Article 28 clicks
Cite This Article 28 clicks













Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.